Patient Faces Life Post-COVID with Help from Post-ICU Recovery Clinic at University Hospitals
July 28, 2022

Program aids patients with Post Intensive Care Syndrome
In December of 2020 Rocco Greco tested positive for COVID-19, but his battle back to “normal” would last months.
Complications landed him in the intensive care unit at a hospital in Warren, Ohio near his home in Cortland.
“I was in bad shape. My son and daughter came to visit to say goodbye. No one thought I was going to make it through the night, but I did,” said Greco.
Greco’s care team decided he should be transferred to University Hospitals (UH), and after a delay because of snowstorm he was flown to UH Cleveland Medical Center.
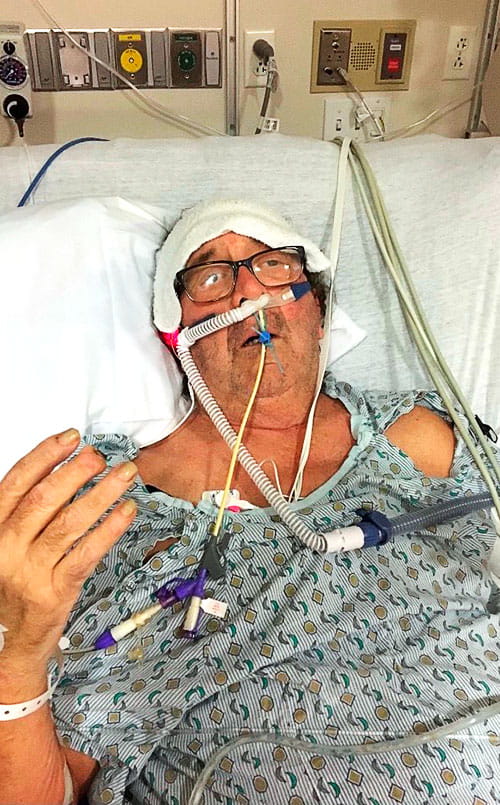
Greco spent 24 days on a ventilator to help him breathe and 40 days in the hospital’s medical intensive care unit or MICU. He finally improved enough to be discharged from UH on Valentine’s Day 2021 but spent some time at a rehabilitation hospital before ultimately returning home.
Although happy and relieved to be home, Greco wasn’t able to return to life as normal before COVID. Many patients who’ve experienced an ICU stay face similar struggles.
ICU patients may suffer from what has become known as Post Intensive Care Syndrome (PICS). The term describes new or worsening deterioration in physical, emotional or cognitive health following a critical illness. Sufferers may have problems thinking clearly, or they may feel a lingering weakness throughout their body. Anxiety and depression can be other after-effects. The condition persists after a patient's discharge from the hospital, when other people in their life like family members or coworkers may view them as “better” or “cured.”
Risk factors for PICS include a patient who has experienced delirium, sepsis and/or acute respiratory distress syndrome (ARDS), a serious lung condition that causes low blood oxygen. Other risk factors are a length of stay in the ICU that lasts more than 72 hours, and being placed on a mechanical ventilator for more than 48 hours.
Studies show that after one year, 50 percent of former ICU patients require caregiver assistance, and 48 percent have not returned to work.
“When someone is discharged from the hospital, they generally expect to be back to normal or close to it – and that’s what the people around them expect, too,” said Janet Kloos, RN, PhD, APRN-CNS at UH Cleveland Medical Center and leader of the UH Post-ICU Recovery Clinic. “But we know that isn’t the case for many people who leave the ICU.”
Greco had been retired from the Ohio Department of Natural Resources for more than a decade, so he didn’t have to worry about going back to work, but he faced other issues.
“I had intestinal problems. I had gained a lot of weight and my blood pressure was high,” said Greco. “But most bothersome was I just didn’t feel like myself. I was having cognitive issues – brain fog – they call it. I felt an anxiety that just wouldn’t go away.”
That’s when Greco was referred to the University Hospitals Post-ICU Recovery Clinic.
The program’s roots go back to 2014, when a support group was established at UH Cleveland Medical Center for post-ICU patients and their families with the goals of helping them through their recovery and inspiring current MICU patients.
In 2016, UH Cleveland Medical Center was one of six international centers awarded a THRIVE grant from the Society of Critical Care Medicine to grow its ICU survivor support group. The program is also one of 37 sites internationally that’s part of the CAIRO Collaborative (Critical and Acute Illness Recovery Organization).
Over the years the program has expanded into what it is today.
An appointment with the UH Post-ICU Recovery Clinic includes:
- Medical exam
- Medication reconciliation
- Occupational therapy
- Physical therapy
- Visit with a social worker
- Time with a chaplain (a unique feature nationally)
- Screening for cognitive/emotional health
The program also includes peer support groups and offers in-person as well as online options.
“The mission of University Hospitals is to heal, to teach and to discover,” said Kloos. “The mission statement of the support group expands on this. We want to heal that which is broken after a complicated ICU stay, teach awareness of post-ICU complications, and discover strength and purpose through peer support.”
Through his participation in the UH Post-ICU Recovery Clinic, Greco found support, empathy, and ultimately, improvement in his symptoms.
“Rocco never stops working to better himself,” said Kehllee Popovich, MSN, ACNP-BC, the nurse practitioner who was one of the providers working directly with Rocco in the clinic. “I witnessed him get up every day with a positive attitude and strive to become healthier. He shines his positive light in this world through his love for his family and his involvement in the community.”

“I got to tell my story, how I survived, and how I took it one day at a time,” he said. “And I listened, too. It’s a feeling you get inside when you know other people have gone through what you went through. You know you’re not the only one and it takes a load off your mind and eases your anxiety.”
Greco, now 67, says he’s at an appropriate weight through improved diet. His brain fog and anxiety have significantly diminished. He writes in his diary every day, plays word games and has started liking to cook. He walks one mile twice daily and has returned to officiating high school volleyball. He loves gardening and maintains hundreds of varieties of day lilies in his yard.
Greco still participates in the Post-ICU Recovery Clinic at UH.
“I enjoy sharing the love. The clinic has helped me get better and I hope I helped some people, too,” he said.


