Novel Biobank Accelerates Fibromuscular Dysplasia Research
January 25, 2021
Initiative marks entry of University Hospitals Harrington Heart & Vascular Institute into personalized risk prediction and genomics
Innovations in Cardiovascular Medicine & Surgery | Winter 2021
A novel biorepository within University Hospitals Harrington Heart & Vascular Institute, based at University Hospitals Cleveland Medical Center, is paving the way for the future of personalized medicine.
Blood samples collected and maintained in the health system’s secure, climate-controlled biobank will aid researchers in unlocking the genetic basis for cardiovascular diseases and provide opportunity for collaboration across academic institutions.
Led by Imran Rashid, MD, cardiologist, University Hospitals and Assistant Professor, Case Western Reserve University School of Medicine, and Sanjay Rajagopalan, MD, Chief of the Division of Cardiovascular Medicine at UH Harrington Heart & Vascular Institute, and Professor at the School of Medicine, the biobank will serve as an essential storehouse for investigation into disease biomarkers and effective therapeutics.
“The Harrington Heart & Vascular Institute Biobank initiative marks the entry of our institute into personalized risk prediction and genomics, which is already shaping medical care in a big way,” Dr. Rajagopalan says.
FIBROMUSCULAR DYSPLASIA STUDIED THROUGH BIOBANK INITIATIVE
 Heather Gornik, MD
Heather Gornik, MDPatients coping with fibromuscular dysplasia (FMD), a non-atherosclerotic disease of the arterial walls, will be invited to participate in the biobank to advance understanding of this idiopathic disease.
“Fibromuscular dysplasia is a rare vascular disease that can have a major impact on patients’ health and quality of life,” says Heather Gornik, MD, a world-renowned expert in FMD who is Co-Director of the Vascular Center and Director of the Fibromuscular Dysplasia and Arterial Dissection Program at UH Harrington Heart & Vascular Institute, and Professor of Medicine at the School of Medicine.
Prior work has shown that there are likely significant genetic underpinnings to the development of FMD, though these are currently poorly understood, Dr. Gornik says. “Developing a biorepository of blood samples from patients with FMD and related conditions, including coronary and cervical artery dissection, will allow us to collaborate with basic and translational scientists to understand further why FMD develops.”
A 500-PATIENT FMD BIOBANK
Patients seen in the FMD and dissection clinic at University Hospitals are among those eligible to participate in the biobanking of blood samples. Currently, the system’s innovative clinical and research program follows approximately 300 patients, many of whom travel from across the country to receive expert care.
With funding from the National Institutes of Health and the UH Harrington Heart & Vascular Institute, the initial goal is to enroll up to 500 patients diagnosed with FMD, spontaneous coronary artery dissection and cervical artery dissection. Blood samples will be processed, frozen and stored in the biobank for ongoing and future research initiatives.
Dr. Gornik and her team will collaborate with colleagues at University Hospitals as well as with Santhi Ganesh, MD, at the University of Michigan on genetic analyses. Additionally, the team will participate in an international consortium of FMD genetics researchers that includes colleagues in France, Belgium and Australia.
“The genetics of FMD are complex, and there may be multiple factors that increase risk of its development,” Dr. Gornik says. “The biobank is but one study in our FMD research program, which includes participation in the United States FMD Registry, the iSCAD Registry and other projects, including an investigation into the prevalence of spine disease among patients with FMD.”
Also of interest are gender prevalence and environmental factors, including hormone therapies, that may contribute to FMD. Approximately 90 percent of patients with FMD are women, although men may present with more aggressive disease, including a higher frequency of aneurysm and dissection.
INTEGRATED EXPERT CARE
The multidisciplinary FMD and Arterial Dissection program at University Hospitals includes collaboration with vascular intervention and vascular surgery, neurointervention and neurosurgery, medical genetics, radiology, and other specialties depending on patient need.
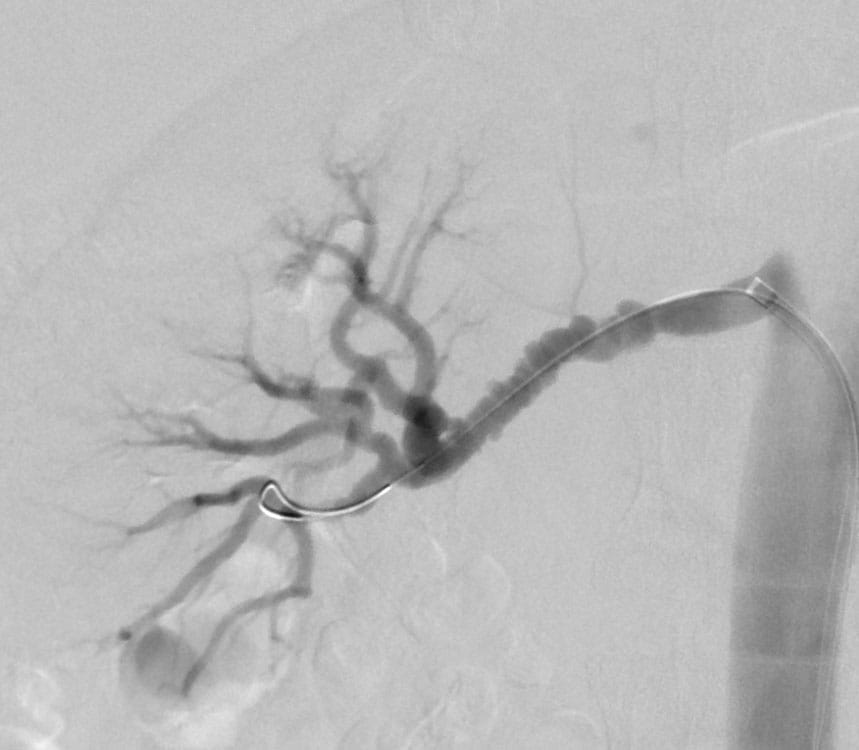 Caption: Shown is the classical "string of beads" of multifocal type FMD in the right renal artery in a patient undergoing an angioplasty procedure for hypertension.
Caption: Shown is the classical "string of beads" of multifocal type FMD in the right renal artery in a patient undergoing an angioplasty procedure for hypertension.A dedicated nurse coordinator, Rebecca Young, RN, BSN, and research coordinators help facilitate personalized care. In addition, information sessions and patient support groups address the psychosocial demands of living with a rare, chronic condition.
Serving as co-chairperson of the 2019 International FMD Consensus, Dr. Gornik is passionate about establishing international guidelines to extend best practices to this underserved patient population across the world.
“With any rare disease, seeing a physician who has cared for hundreds and hundreds of patients provides a different experience and perspective,” she says. “I think patients come to us for that experience. However, we are highly committed to not only caring for our patients with FMD but also learning as much as possible to disseminate that knowledge, so that perhaps someday providers across the country are comfortable recognizing and caring for patients with FMD.”


