Center for Comprehensive Venous Care Offers Advanced Vein Imaging and Therapies
June 21, 2021
New unit at UH Harrington Heart & Vascular Institute leads with advanced imaging and therapies
Innovations in Cardiovascular Medicine & Surgery | Summer 2021
The newly minted Center for Comprehensive Venous Care (CCVC) within University Hospitals Harrington Heart & Vascular Institute offers a full scope of venous care services under the direction of Karem Harth, MD, MHS, a vascular surgeon at University Hospitals Cleveland Medical Center.
 Karem Harth, MD
Karem Harth, MD“I am excited to build a center that leads the way with advanced imaging and therapies to treat a broad range of venous conditions and fosters relationships with practitioners who have a similar passion for venous care,” says Dr. Harth. “Additionally, the center will align services across the healthcare system and include vascular surgery, cardiology, vascular medicine, radiology and wound centers.”
The CCVC will offer a broad range of services for varicose veins and management of leg swelling. Both medically indicated and cosmetic services will be available on an ambulatory basis. Additionally, endovenous therapies for conditions such as acute and chronic deep vein thrombosis (DVT), complex inferior vena cava (IVC) filter retrieval, IVC reconstruction and Pelvic Congestion Syndrome (PCS) will be offered.
Dr. Harth hopes to extend outreach and education regarding management of PCS and chronic DVT. PCS is a chronic condition that can result in unrelenting pelvic pain and morbidity.
“There are multiple causes of pelvic pain,” she says. “However, in my experience, PCS is often poorly understood and overlooked. Patients may go undiagnosed and may end up with the incorrect therapies with little to no relief.”
PCS diagnosis and treatment
An important component of PCS education includes understanding the appropriate pathologic terminology that describes the process leading to the clinical symptoms of PCS. PCS of venous source is best understood as derived from Pelvic Venous Insufficiency (PVI). Though PVI is generally associated with women, the condition can also affect men. Similar to varicose veins visible in the legs, PVI occurs deep within the abdominal and pelvic veins and can be debilitating. Most commonly affecting the ovarian or gonadal vein, valvular reflux and subsequent insufficiency cause veins to become dilated, tortuous and painful.
Effective treatment begins with a complete clinical history. The first step is to understand patient symptoms, risk factors and possible contributors to the unresolved pain. Once there is suspicion of pelvic venous insufficiency, the patient undergoes a duplex ultrasound.
“We take standard pelvic venous evaluation a step further and perform detailed evaluation of the venous beds commonly associated with PVI,” Dr. Harth says. “The studies give us beautiful images in a non-invasive fashion.” Additionally, MRI with angiography can also provide detailed anatomic imaging to assist in determining appropriate therapy options.
For many patients, embolizing the affected vein using a combination of sclerosing agents and endovascular coils is necessary and successful. This outpatient intervention is generally well-tolerated, and patients frequently experience symptom improvement soon after the procedure. In other cases, where the pelvic congestion is due to obstructive venous disease, such as May-Thurner Syndrome, stenting may be required.
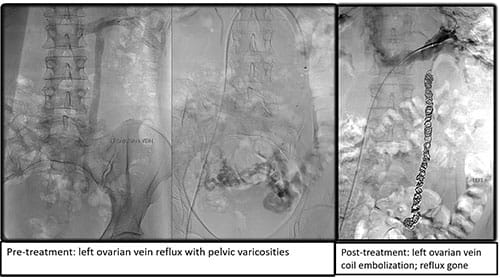 Left ovarian vein coil embolization.
Left ovarian vein coil embolization.“The management of chronic pelvic pain is not straightforward,” Dr. Harth says. “Often, one therapy session is sufficient, but we prepare for the possibility of staging additional interventions. If one intervention is sufficient to achieve pain-free quality of life, then we consider this a success and continue long-term follow-up.”
In addition to developing protocols to expand and standardize PVI care, Dr. Harth and her colleagues are planning a series of talks aimed at raising awareness for both providers and patients at women's and men's health centers and primary care practices. “Endovascular therapy (EVT) for pelvic congestion is not familiar to all referring providers, so it is understandable that patients are not referred for this evaluation” she says. “Helping people find relief is one of the most rewarding aspects of my practice, and my goal is to bring these therapies forward to help more patients return to a better quality of life.”
Investigating chronic DVT
Another condition treated within the CCVC is DVT. Approximately half of patients with DVT develop post-thrombotic syndrome (PTS), experiencing symptom burden that includes leg pain, swelling, heaviness and — in very advanced cases — ulceration.
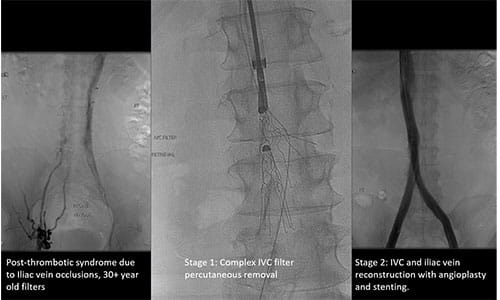 Complex IVC filter removal with IVC and Iliac Vein Reconstruction.
Complex IVC filter removal with IVC and Iliac Vein Reconstruction.UH Cleveland Medical Center, with Dr. Harth as the local Principal Investigator, is participating in the C-TRACT Trial, a randomized study funded through the National Institutes of Health's National Heart, Lung, and Blood Institute (NHLBI) that seeks to determine whether catheter-assisted EVT is effective in reducing the severity of PTS in eligible patients.
“There are a number of studies that suggest there is a benefit to recanalization of the iliac vein via stent placement as compared to standard medications, compression therapy and wound care, but there is no definitive data,” Dr. Harth says. “We are excited to be the only site in our region recruiting patients for this pivotal study of PTS best-practices care.”
For more information or to learn about study eligibility, please contact Dr. Harth at 216-844-3013 or Karem.Harth@uHhospitals.org.
Contributing Expert:
Karem Harth, MD, MHS
Vascular Surgeon
UH Harrington Heart & Vascular Institute
Assistant Professor
Case Western Reserve University School of Medicine


