UH Launches HIPEC Program for Ovarian Cancer
October 07, 2020
Gynecologic oncology and surgical oncology join effort to provide new treatment that can improve survival times
Innovations in Obstetrics & Gynecology | Fall 2020
 Christa Nagel, MD
Christa Nagel, MDUniversity Hospitals has spent the past six months preparing to offer hyperthermic intraperitoneal chemotherapy (HIPEC) to ovarian cancer patients. Now, UH is officially launching the program through the collaborative efforts of its gynecologic oncologists and surgical oncologists. This additional treatment is targeted to patients after surgical removal ovarian tumors. HIPEC involves irrigation of the abdominal cavity with heated chemotherapy agents that target small to microscopic tumor cells that may remain behind after surgery.
Christa Nagel, MD, Gynecologic oncologist at University Hospitals Cleveland Medical Center and University Hospitals Seidman Cancer Center and an Assistant Professor of Gynecologic Oncology at Case Western Reserve University School of Medicine, discusses why UH decided to pursue the HIPEC program and how it can help patients.
A PROGRAM BACKED BY EXPERIENCE AND CLINICAL EVIDENCE
While HIPEC for ovarian cancer is a new offering at UH, the healthcare system and Dr. Nagel are experienced in this treatment approach for other conditions, such as appendiceal cancer. Dr. Nagel worked with HIPEC during her fellowship training at the University of Texas Southwestern Medical Center. When she arrived at UH, she worked with surgical oncologist John Ammori, MD, Program Director of General Surgery at UH Cleveland Medical Center and Associate Professor at the School of Medicine.
“People have tried [HIPEC] on and off for ovarian cancer probably over the last 10 years,” Dr. Nagel says. “It wasn’t until a couple years ago, when a large trial came out that showed that HIPEC chemotherapy had a survival benefit for people who were also being treated with neoadjuvant chemotherapy.”
The 2018 study published in The New England Journal of Medicine demonstrated that stage III epithelial ovarian cancer patients treated with interval cytoreductive surgery and HIPEC had longer survival times than patients treated with surgery alone.
“We waited for the data to mature,” Dr. Nagel says. “UH has decided this an important treatment option to offer our patients now that there is a study that shows a survival benefit.”
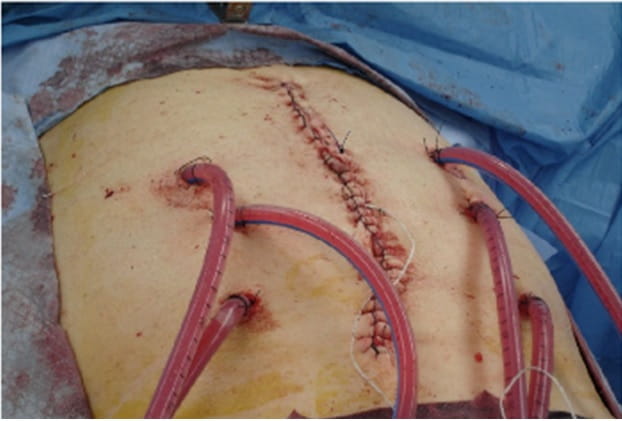 HIPEC intraoperative set-up at the time of interval debulking for advanced ovarian cancer.
HIPEC intraoperative set-up at the time of interval debulking for advanced ovarian cancer.Over the past six months, UH has developed protocols for the HIPEC program for ovarian cancer. The addition of HIPEC extends surgery time by about two hours, according to Nagel. The procedure also requires the support of a perfusionist to run the machine that cycles the chemotherapy drugs through the patient’s body and an anesthesiologist.
The program has just launched at UH through the joint efforts of the Gynecologic Oncology and Surgical Oncology. For now, it will focus on interval debulking for advanced ovarian cancer.
FURTHERING INNOVATION IN GYNECOLOGIC ONCOLOGY
The new HIPEC offering for ovarian cancer is just one way UH demonstrates its commitment to innovative patient care. “It requires a lot of time and resources in order to implement a program like this,” Dr. Nagel says.
“UH sees the value in anything that increases prognosis and survival and the ability to care for patients with these types of advanced cancers.”
In addition to this program, Dr. Nagel is pursuing other research avenues for ovarian cancer treatment. One of her research pursuits is in platinum refractory ovarian cancer. UH is currently involved in a trial focused on patients who have been off of platinum-based chemotherapy for less than six months and have a recurrence of their cancer. “These patients tend to have a poor prognosis,” she says. “That is why this is a passion of mine. it is our goal and hope to increase survival rates and time and improve their prognosis.”
To learn more about how UH is leveraging HIPEC for patients with ovarian cancer, please call 216-553-1537.


