UH Digestive Health Institute Physicians Advance Promising Clinical Trial for Pancreatic Cancer Patients
February 18, 2019
A new drug may benefit patients with locally advanced or borderline resectable pancreatic cancer
Innovations in Digestive Health – Winter 2019
University Hospitals Seidman Cancer Center, with Case Comprehensive Cancer Center, is currently recruiting for a Phase II single-arm clinical trial to study the effects of CPI-613, a drug in development by Rafael Pharmaceuticals, in combination with standard-of-care FOLFIRINOX. Jordan Winter, MD, Chief of Surgical Oncology for UH Cleveland Medical Center, authored the trial.
A Phase I study showed encouraging results in patients with metastatic pancreatic cancer: three complete responses to the drug — when used in combination with FOLFIRINOX — out of 18 patients, for a 17 percent complete response rate. The overall response rate was 61 percent.
Principal investigator for the UH Phase II trial, Jeffrey Hardacre, MD, FACS, Interim CMO for University Hospitals Seidman Cancer Center, Chief Surgical Quality Officer, University Hospitals Digestive Health Institute; and Professor of Surgery for Case Western Reserve University School of Medicine, says study participants in the Phase I trial also survived longer than expected with FOLFIRINOX alone.
 Jeffrey Hardacre, MD
Jeffrey Hardacre, MD“Because there was such a positive signal in patients with metastatic pancreatic cancer, we want to see if there’s a similar signal in patients with locally advanced or borderline resectable cancer when compared to controls,” he says. “If we see those positive signals, we’ll advance to Phase III trials.”
CPI-613 targets enzymes in mitochondria involved in cancer cell energy. The drug’s attack on metabolic activity increases the sensitivity of cancer cells to diverse chemotherapeutic agents.
The Need For More Treatment Option
The American Cancer Society estimates about 56,770 Americans will be diagnosed with pancreatic cancer in 2019. The five-year survival rates for Stage IA and IB pancreatic cancer is only 14 and 12 percent, respectively.
“We need a more reliable method of early detection and better forms of nonsurgical therapy,” Dr. Hardacre says. “Improvements in chemotherapy and immunotherapy will allow us to have a greater impact on a broader group of patients.”
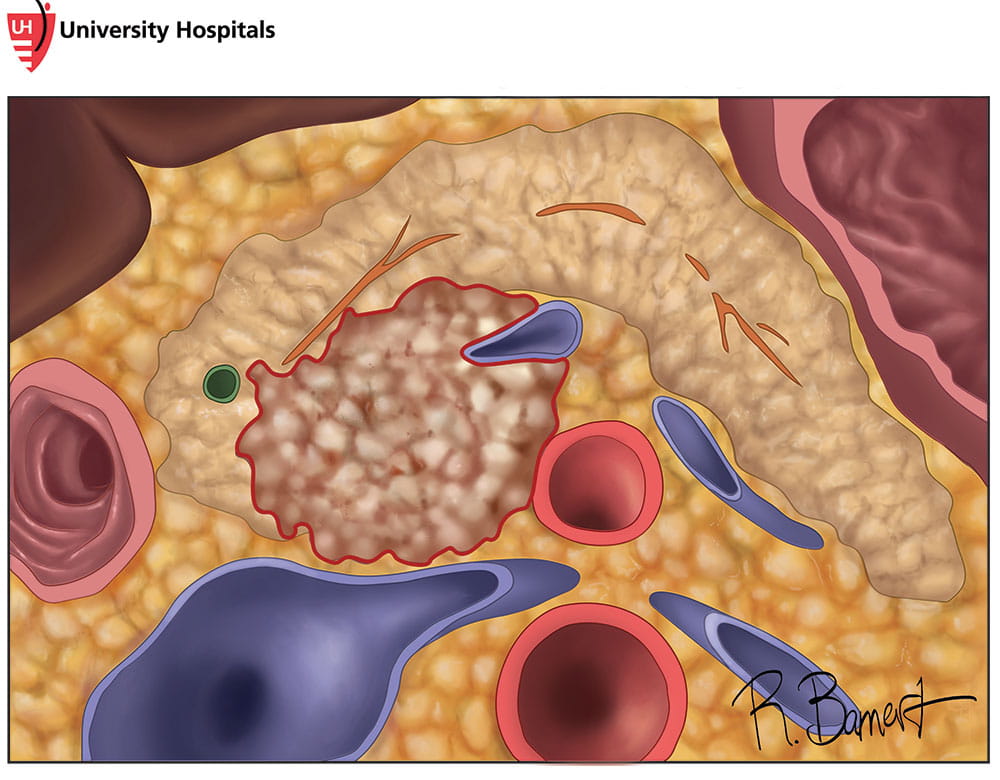
For some pancreatic cancer patients, these treatments precede surgery. Increasingly, oncologists recommend neoadjuvant therapy — chemotherapy, radiation therapy or other therapy given before surgery — to treat certain pancreatic cancers.
CP-613 Trial Still Recruiting
“After major operations, some patients don’t recover well enough to tolerate postoperative therapy,” Dr. Hardacre explains. “If we give therapy before surgery, they’re more likely to get combined modality therapy, because they’ll receive chemotherapy when they’re in better shape.”
Phase III trials have shown adjuvant chemotherapy improves five-year survival in resectable pancreatic cancer. However, between 30 and 50 percent of eligible patients don’t actually receive it, mainly due to postoperative complications. Neoadjuvant therapy not only ensures patients receive full treatment, it targets cancer-initiating cells early, which may increase survival.
Dr. Hardacre says his team is still recruiting patients for the CP-613 clinical trial. “We’re happy to evaluate patients with non-metastatic locally advanced pancreatic cancer to see if they’re eligible.”
Because it’s an aggressive treatment, he says patients must be in relatively good health to tolerate the regimen. For inclusion criteria, refer to NCT number NCT03699319 at ClinicalTrials.gov.
“This study is looking at a drug that, in preliminary analysis, is shown to be favorable with metastatic pancreatic cancer,” Dr. Hardacre says. “We’re optimistic that we’ll see positive signals with locally advanced or borderline resectable cancers.”
To refer a patient for clinical trial evaluation, call 800-641-2422.


