Central Sleep Apnea: Challenging to Manage
June 02, 2019
UH investigates new CSA treatments to improve patient outcomes
Innovations in Pulomonogy and Sleep Medicine | Summer 2019
For patients with central sleep apnea (CSA) due to Cheyne-Stokes breathing, there are no good treatment options, says Ambrose A. Chiang, MD, FCCP, FAASM, Director of Sleep Medicine at University Hospitals Cleveland Medical Center. UH is hoping to help change this.
 Ambrose Chiang, MD
Ambrose Chiang, MDLOFT-HF CLINICAL TRIAL
Cheyne-Stokes breathing is an abnormal periodic breathing pattern with recurrent central sleep apneas. About half of patients with congestive heart failure with low left ventricular ejection fraction (LVEF) may have significant Cheyne-Stokes breathing, which has a poor outcome and is difficult for physicians to treat.
“Studies suggest that when patients have Cheyne-Stokes breathing, they have a two-fold increase in mortality,” Dr. Chiang says.
UH is actively recruiting patients for LOFT-HF — The Impact of Low Flow Nocturnal Oxygen Therapy on Hospital Admissions and Mortality in Patients with Heart Failure and Central Sleep Apnea. LOFT-HF is a Phase III, multi-center, randomized, double-blind, sham-controlled, outcomes trial.
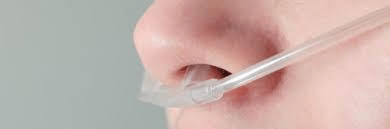 The LOFT-HF clinical trial will evaluate the long-term effects of nocturnal oxygen therapy in certain patients with heart failure and CSA-Cheyne-Stokes breathing.
The LOFT-HF clinical trial will evaluate the long-term effects of nocturnal oxygen therapy in certain patients with heart failure and CSA-Cheyne-Stokes breathing.Patients enrolled in LOFT-HF will be randomized for oxygen therapy or sham oxygen therapy. The composite primary outcome is the first occurrence of either mortality due to any cause, a life-saving cardiovascular intervention or an unplanned hospitalization for worsening heart failure measured over the duration of the trial. Patients will be followed for an average of 2.5 years.
According to Dr. Chiang, Continuous Positive Airway Pressure (CPAP), the standard treatment for obstructive sleep apnea, was used for many years as a treatment for patients with Cheyne-Stokes breathing. Unfortunately, a controlled clinical trial later failed to show significant benefit with CPAP in these patients. The CANPAP trial (Canadian Continuous Positive Airway Pressure for Patients with Central Sleep Apnea and Heart Failure), published in 2005, found that CPAP did not affect overall survival, quality of life or hospitalization in patients with predominantly CSA and congestive heart failure with low LVEF.
Then, in 2006, Adaptive Servo Ventilation (ASV), an innovative positive airway pressure device, became available to sleep physicians for treatment of CSA.
“We were very excited about this technology,” Dr. Chiang says. “It really seemed to normalize the breathing in sleep in those with Cheyne-Stokes breathing.”
However, in 2015, the SERVE-HF trial demonstrated that ASV not only failed to improve the study composite primary endpoint, but instead, significantly increased cardiovascular and all-cause mortality. The American Academy of Sleep Medicine swiftly advised physicians to stop using ASV in patients with low LVEF and predominantly CSA within a week after ResMed, an ASV manufacturer, sent a field safety notice to sleep physicians.
Sleep physicians like Dr. Chiang are now hoping that the results of LOFT-HF will change the treatment paradigm for patients with CSA.
If you have patients with Cheyne-Stokes Breathing and LVEF less than 45 percent as demonstrated on an echocardiogram or other imaging methods, you can refer them to UH for enrollment in LOFT-HF. Call Dr. Chiang’s office at 216-844-3201, leave your patient’s phone number and UH will contact the patient.
LOFT-HF Phase III Clinical Trial
PIs at UH: Drs. Ambrose Chiang and Guilherme Oliveira
Subjects: 858 patients at 40 centers in United States and Canada
Data Coordinating Center: Brigham and Women's Hospital/Harvard Medical School
Clinical Coordinating Center: The Ohio State University College of Medicine
Funding: National Institutes of Health
REMEDE
Since CSA is difficult to treat and leads to poor outcomes, UH is committed to finding new and effective ways to help these patients. To that end, UH hopes to offer the Remede device later this year.
Remede is a transvenous phrenic nerve stimulation device and a potential treatment option for patients with moderate to severe central sleep apnea due to Cheyne-Stokes breathing. It uses an implanted, battery-powered pulse generator that is controlled by an external, portable tablet programmer. During the implant procedure, a cardiac electrophysiologist implants thin wire leads that will deliver small electrical pulses to the phrenic nerve, which stimulates breathing while the patient is sleeping.
“Many of these patients are simply hard to treat,” Dr. Chiang says. “Several studies showed that CSA can be a lot better controlled with this device. We’re in the process of forming a Remede team and hoping we can provide this device to our UH patients soon.”
For more information about central sleep apnea, the LOFT-HF trial or Remede, call Dr. Chiang at 216-844-3201.


