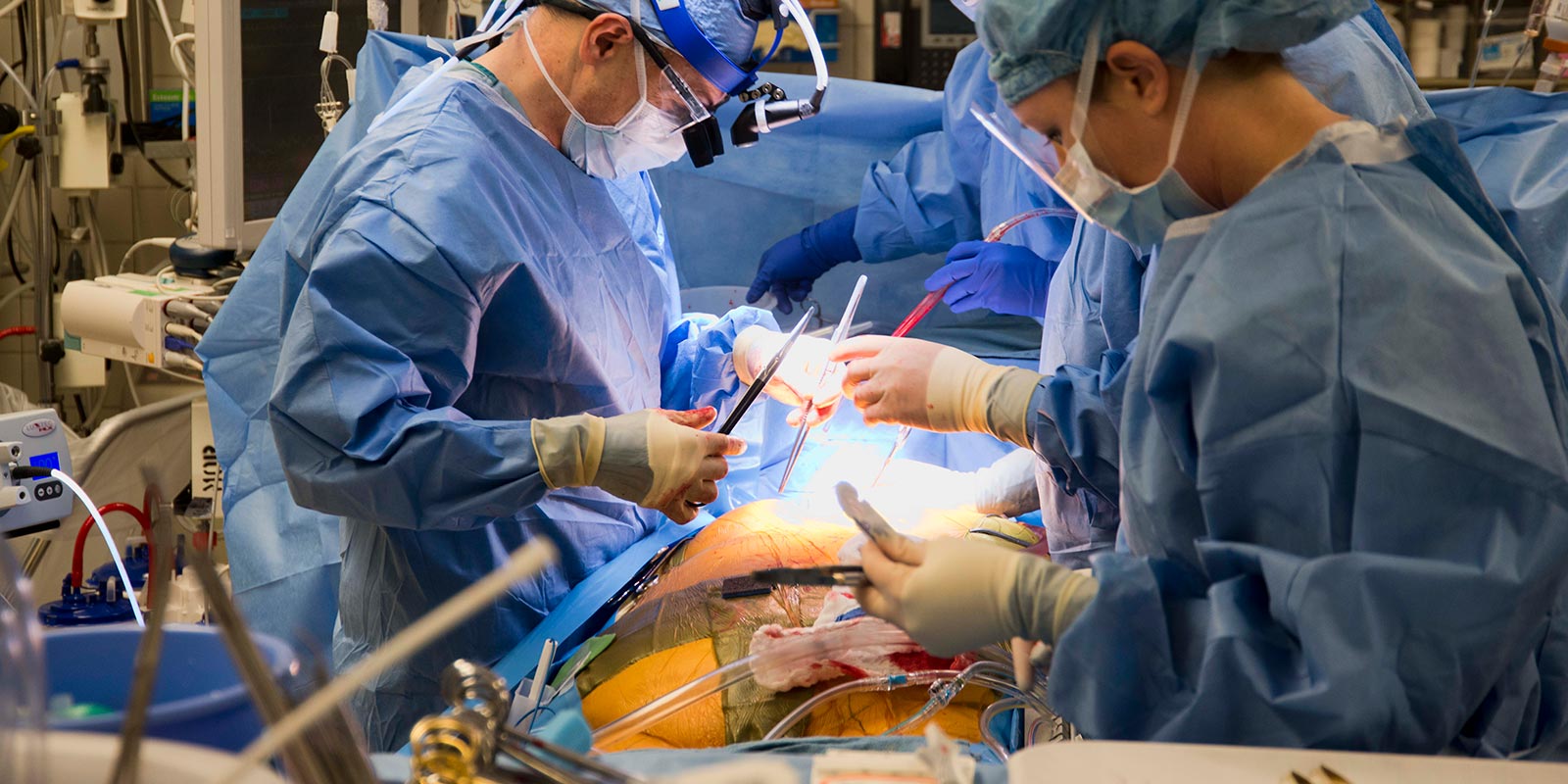
Surgical Ablation Options for Atrial Fibrillation (AFib)
Surgical ablation creates scar tissue in the heart to block the electrical signals that trigger AFib. It’s used for persistent or longstanding AFib that hasn’t improved with medication or catheter ablation, or when symptoms return. University Hospitals Harrington Heart & Vascular Institute offers three surgical approaches – Maze, mini-Maze and convergent – tailored to each patient’s needs and offering some of the best success rates for managing AFib.
Your heart health is important. Don’t delay care.
Call 216-844-4004 to schedule an appointment with a UH cardiac surgeon.
Quick Facts
- What it is: Unlike catheter ablation, a surgical ablation is a surgical technique that creates permanent scar lines in the heart to block irregular electrical signals and restore the heart’s normal rhythm.
- Who it’s for: Patients with persistent AFib that hasn’t responded to medications, catheter ablation or electrical cardioversion, or those already undergoing cardiac surgery for another reason.
- Types: Maze is a traditional open approach with a larger incision. Mini-Maze uses small incisions and video guidance to accomplish the same goal with less trauma. Convergent combines surgical and catheter ablation in one procedure to target AFib more completely.
- Success highlights: Offers some of the best long-term success rates for staying in normal rhythm; many patients can reduce or stop antiarrhythmic medications completely.
- Recovery snapshot: Hospital stay is typically 1-3 days; return to normal activities in 4 – 8 weeks depending on procedure type and extent of surgery.

What Does Surgical Ablation Do for AFib?
Surgical ablation is a rhythm-control procedure where a cardiac surgeon creates precise lines of scar tissue in the heart to block the electrical signals that trigger AFib. It’s used for patients whose AFib hasn’t improved with medication or catheter ablation, or when open heart surgery is already planned for another condition (like bypass or valve repair). By restoring a more normal heart rhythm, surgical ablation aims to reduce the need for lifelong medication.
Who Is a Candidate for Surgical Ablation?
You may be a good candidate for surgical ablation if you have:
- Persistent or longstanding AFib that hasn’t responded to antiarrhythmic medications.
- AFib that returned after a previous catheter ablation procedure.
- Enlarged atria or complex rhythm patterns that make catheter ablation less likely to succeed.
- Another heart condition (such as valve disease or coronary artery disease) that requires open-heart valve or bypass surgery.
- Bothersome AFib symptoms affecting your quality of life despite treatment attempts.
Not sure if you’re a candidate?
Your UH cardiologist or electrophysiologist can evaluate your AFib type, heart anatomy, overall health and treatment history to determine if surgical ablation is right for you. Schedule a consultation to discuss your options.

Who is a candidate for the convergent procedure?
The convergent procedure is ideal for patients with symptomatic, persistent AFib that hasn’t improved with medication, or those who have had one or more catheter ablation procedures that failed. It’s also a good option for patients who want AFib treatment but are unable to tolerate the larger incisions and longer recovery of open-heart surgery. Unlike traditional Maze surgery, convergent candidates typically do not need other open-heart procedures at the same time.
How the convergent procedure works
The convergent procedure combines minimally invasive surgical ablation on the outside of the heart with catheter-based ablation on the inside, performed by a cardiac surgeon and electrophysiologist working as a team. Small incisions allow the surgeon to access the heart’s outer surface and create scar lines that block abnormal electrical signals. At the same time, the electrophysiologist uses catheter techniques to ablate from inside the heart, targeting additional AFib triggers. This combined approach treats AFib more completely than either technique alone.
Convergent procedure success and recovery
The convergent procedure achieves freedom from AFib in up to 85 percent of patients, though results vary depending on AFib type, heart structure and individual factors. Most patients stay in the hospital overnight and return to normal activities faster than those undergoing traditional open Maze surgery, typically resuming work and exercise within 3 – 4 weeks.
Surgical Maze Procedure and Recovery: What to Expect
The Cox-Maze IV procedure is the original surgical ablation approach for treating AFib. It uses radiofrequency or cryoenergy to create a precise “maze” of scar lines in the heart’s upper chambers, blocking the electrical signals that trigger AFib. The procedure includes left atrial appendage (LAA) closure to reduce stroke risk.
- When Cox-Maze IV is recommended
-
Cox-Maze IV is typically recommended for patients who need open-heart surgery for another reason, such as valve repair or replacement, or coronary bypass, and also have AFib. It’s also an option when other rhythm-control treatments (medication or catheter ablation) have not been successful or are not possible.
- How Maze surgery is performed
-
During the procedure, the surgeon opens the chest to access the heart and uses radiofrequency (heat) or cryoenergy (cold) to create lines of scar tissue in the atria. These scar lines form a “maze” pattern that blocks the abnormal electrical signals causing AFib. The surgeon also closes the LAA, a small pouch where blood clots commonly form in AFib patients. Studies show that LAA closure in appropriate candidates can reduce stroke risk by more than 90 percent.
- Maze success and recovery
-
- During Surgery: The procedure is performed under general anesthesia with a heart-lung machine. The surgeon makes an incision to open the chest, applies energy to create scar lines and closes the LAA.
- Hospital Stay: Most patients require hospitalization for 3-5 days, often in the intensive care unit, depending on procedure complexity and whether other heart surgery was performed at the same time.
- Initial Recovery: After surgery, patients are monitored closely. Pain is typically managed with medications, and activity is gradually increased. Wound care includes keeping the incision clean and dry. Most patients can resume light activities within 2-3 weeks and return to normal routines within 6-8 weeks with physician clearance.
- Long-Term Follow-up: Your care team will monitor your heart rhythm with office visits and periodic heart monitoring. If surgery successfully restores normal rhythm, blood thinners may be discontinued several months after surgery based on your individual stroke risk and rhythm status.
How to Prepare for a Surgical Ablation Procedure
Your surgical team will take a comprehensive medical history, perform a complete physical exam and order tests to ensure you’re healthy enough for surgery. Your surgeon will also review your medications and provide detailed pre-operative instructions, including when to stop eating and drinking.
Common pre-surgery tests:
- Blood tests to check kidney function, liver function, and blood clotting
- Chest X-ray to evaluate lung health
- Electrocardiogram (EKG) to assess heart rhythm
- Echocardiogram (heart ultrasound) to evaluate heart structure and function
If you take blood thinners, your surgeon will provide specific instructions on when to stop or adjust them before surgery. It’s very important to follow these instructions exactly to balance bleeding risk during surgery with stroke prevention.
Recovering From AFib Surgery
Surgical ablation typically takes 2 – 4 hours, followed by close monitoring in the intensive care unit (ICU) for at least 1 – 2 days. Hospital stays can range from overnight for convergent procedures to one week or longer for traditional open Maze surgery.
You’ll spend time in the intensive care unit or recovery room with close monitoring. Most patients stay in the hospital for 3 – 5 days. Your surgical team will monitor your heart rhythm and manage pain with medications. Activity increases gradually at home, with full recovery typically taking 6 – 8 weeks.
What to expect after AFib surgery:
- Pain and fatigue: Some pain and incision discomfort are normal; your doctor will prescribe pain medications as needed. Feeling unusually tired is also normal and typically improves over several weeks.
- Activity restrictions: Avoid heavy lifting, strenuous exercise and driving for 4 – 6 weeks. Gradually increase activity as tolerated, following your surgeon’s specific guidance.
- Incision care: Keep the incision clean and dry. Your care team will provide detailed wound care instructions and watch for signs of infection.
- When to call your care team: Contact your surgeon if you notice fever, increasing redness or swelling at the incision, chest pain, shortness of breath, or irregular heartbeats.
Most patients return to normal activities within 8 – 10 weeks, though individual timelines vary based on procedure type and overall health.
If your heart rate is too slow after surgery (post-operative bradycardia), your doctor may recommend a temporary or permanent pacemaker to help you maintain an adequate heart rate during healing.
Most patients return to normal activities within 8 – 10 weeks, though individual timelines vary based on procedure type and overall health.
If your heart rate is too slow after surgery (post-operative bradycardia), your doctor may recommend a temporary or permanent pacemaker to help you maintain an adequate heart rate during healing.
Comparing Surgical Ablation Types
| Type | How It’s Performed | When It’s Considered |
|---|---|---|
| Maze | Open-heart surgery with larger incision | When you already need heart surgery for another reason |
| Mini-Maze | Minimally invasive with small incisions | Persistent AFib that hasn’t improved with other treatments |
| Convergent | Combined surgical and catheter approach | Failed catheter ablation or complex AFib patterns |
How Does Surgical Ablation Compare to Catheter Ablation?
Catheter ablation and surgical ablation are both rhythm-control procedures, but they differ significantly in how they are performed.
Catheter ablation is minimally invasive – performed through small tubes (catheters) threaded through blood vessels – and is often a first-line treatment for AFib. Surgical ablation involves creating scar tissue through a surgical approach. It is typically recommended if catheter ablation hasn’t worked or isn’t possible due to heart anatomy, or when you’re already undergoing open-heart surgery for another reason.
Recovery after each approach is also different. Catheter ablation patients usually go home the same day or after an overnight stay, while surgical ablation recovery ranges from overnight (minimally invasive approach) to one week or longer (open-chest Maze approach).
In some cases, surgeons and electrophysiologists may combine both approaches, performing catheter ablation and surgical ablation in the same procedure — known as a convergent approach — to treat complex AFib more completely.
Frequently Asked Questions About Surgical Ablation
- Is surgical ablation considered major surgery?
-
Surgical ablation can range from minimally invasive (small incisions) to open-heart surgery, depending on the procedure type and your clinical needs. Mini-Maze and convergent procedures are less invasive than traditional Maze surgery.
- How long is recovery after surgical ablation?
-
Recovery varies for each approach. Minimally invasive procedures often involve shorter recovery (3 – 4 weeks), while open-chest Maze procedures require longer healing (8 – 10 weeks) and a brief hospital stay.
- Is surgical ablation permanent?
-
The scar tissue created during surgical ablation is permanent – it doesn’t go away. However, the results vary. Many patients stay free from AFib long-term, while others may still have occasional episodes or continue needing medications. AFib can sometimes return, or new problems with rhythm can develop over time.
- Who is a candidate for surgical ablation?
-
Candidates often include patients with persistent or longstanding AFib, enlarged atria, unsuccessful prior catheter ablation or those already undergoing cardiac surgery for another reason. Your surgeon will evaluate your individual situation.
- How painful is surgical ablation?
-
Pain levels depend on the surgical approach. Minimally invasive procedures typically involve less discomfort, while open-chest procedures require more recovery time and incision care. Your surgical team will manage pain with medications as needed.
Learn More & Schedule an Appointment

Choosing a Cardiac Electrophysiologist
Cardiac electrophysiologists (EPs) are cardiologists with advanced training in diagnosing and treating heart rhythm disorders like atrial fibrillation (AFib), atrial flutter and other arrythmias. University Hospitals Harrington Heart & Vascular Institute offers integrated EP, cardiology and surgery care with access to advanced treatment options.


