
Compassionate, Comprehensive Care for Patients with COVID Long-Haul Syndrome
Recent studies have shown that 20 – 30 percent or more of individuals infected with COVID-19 will continue to have health problems for weeks, even months, after their body has cleared the virus. The University Hospitals COVID Recovery Clinic is dedicated to the comprehensive evaluation, diagnosis and multidisciplinary treatment of patients with Post-Acute Sequelae of SARS-CoV-2 infection (PACS), more commonly referred to as COVID Long-Haul Syndrome.
Schedule an Appointment
If, after your acute course of COVID-19, you are still experiencing symptoms, call us today at 216-966-9000 to schedule an evaluation.Advanced Multidisciplinary Expertise for Optimal Outcomes
Patients with COVID Long-Haul Syndrome often seek medical help but their symptoms are not recognized as being COVID-related, so they don’t receive the coordinated, multidisciplinary care they need. At the UH COVID Recovery Clinic, patients have access to a vast network of medical specialists with the training and experience to recognize the syndrome, perform the appropriate diagnostic tests, and develop a personalized treatment plan to address every physical and behavioral aspect of the patient’s illness, which may include the following symptoms:
- Shortness of breath, coughing and fever
- Fatigue and exhaustion
- Brain fog
- Atypical chest pain and palpitations
- Behavioral health issues like depression and anxiety
- Difficulties with cognition and memory
- Insomnia and other sleep problems
- Generalized pain and muscle aches
- Joint pain and impaired mobility
- Persistent loss of smell and taste
- Headache
- Diarrhea
- Skin rashes
The multitude of complaints listed above reflect how COVID Long-Haul Syndrome can affect multiple organ systems in the body, including the pulmonary, hematologic, cardiovascular, neuropsychiatric, renal, endocrine, gastrointestinal/hepatobiliary and dermatologic systems. The impact on patients’ health can range from mild to severe with the latter being totally debilitating.

Creating Personalized Pathways to Healing
Located at UH Ahuja Medical Center, the UH COVID Recovery Clinic offers both in-person and virtual care based on the patient’s specific symptoms and needs. Our goal is to identify the best way(s) to manage your symptoms and coordinate the multidisciplinary care required to restore your health. Care will be individualized for you as a whole person - both mind and body - and designed to help you return to the activities you love. Patients can schedule an appointment directly with the UH COVID Recovery Clinic or may be referred for an evaluation by their primary care provider.
Scheduling Appointments and Medical Questionnaires
Once you have scheduled an appointment, you will be emailed or mailed a medical questionnaire to complete and send back. This questionnaire will ask you to provide details about your COVID history (dates, symptoms and treatments received) along with a description of your current symptoms and other health issues as compared to your functioning status prior to COVID.
Once we have your completed questionnaire, the patient journey will be as follows:
Initial Assessment
At the initial evaluation (in person or virtually) you will meet with our specially trained nurse practitioner who will review your questionnaire and ask additional questions designed to screen for depression, anxiety, sleep disturbances, fatigue, cognitive deficits and more. You will also be asked about your current symptoms, day-to-day activities, medical history and the medications you are taking. For those being seen in person, the nurse practitioner will perform a physical examination.
Based on the findings of the initial assessment, the nurse practitioner, in collaboration with the UH COVID Recovery Clinic’s medical director, David M. Rosenberg, MD, MPH, will develop a care path for each patient. This care path will often include input from individual members of our multispecialty panel. Your care will be approached as a team effort in order to guide your pathway to recovery.
Personalized Diagnostic Testing
An accurate diagnosis is essential for a successful treatment plan. Based on the information collected during the initial assessment, and on the recommendation of the specialists on the patient’s care team, a variety of diagnostic tests may be ordered. These may include but are not limited to:
- Pulmonary function testing
- Imaging tests that may include computed tomography (CT) scans and magnetic resonance imaging (MRI)
- Cardiovascular testing including electrocardiogram (EKG) and/or event monitoring, echocardiogram, stress testing
- Laboratory testing
- Sleep studies
- Neuropsychological testing
- Testing for autonomic dysfunction
Collaborative, Multidisciplinary Team Approach to Care
Based on the patient’s specific symptoms and the care plan developed by the nurse practitioner and medical director, referrals for specialty consultation may be deemed appropriate. These types of referrals will help customize the treatment team for a given patient. Potential specialty areas for referral include:
- Pulmonary
- Pulmonary
- Heart & Vascular
- Sleep Medicine
- Behavioral & Integrative Health
- Neurology & Neuropsychology
- Rheumatology, Infectious disease & Immunology
- Otolaryngology (ENT)
- Digestive health
- Endocrinology/Metabolic Health
Treatment Plan and Follow-Up Care
Your on-going care surrounding COVID will be managed by your team at the UH COVID Recovery Clinic and regular follow-ups with our nurse practitioner will be scheduled. The nurse practitioner will help coordinate recommendations received by your care team, namely that provided by given specialists or those providing specific treatment. All information pertaining to your care surrounding COVID will be forwarded directly to the UH COVID Recovery Clinic’s electronic data base, ensuring that our staff is always up-to-date on the care you have received.
To monitor and track your progress over time, we will occasionally ask you to update us with details about your treatment, symptoms and overall path to recovery. Your team at the UH COVID Recovery Clinic will use this data to help define the natural history of COVID Long-Haul Syndrome and advance much-needed research related to the diagnosis, symptoms and treatments for this syndrome.
COVID-19 Recovery & Longhauler Clinical Study
The University Hospitals Clinical Research Center is conducting an observational research study about COVID-19 (also known as SARS-CoV2) to learn more about long-term effects of COVID-19, and who is at greatest risk. To learn more, visit the COVID-19 Recovery & Longhauler Study.
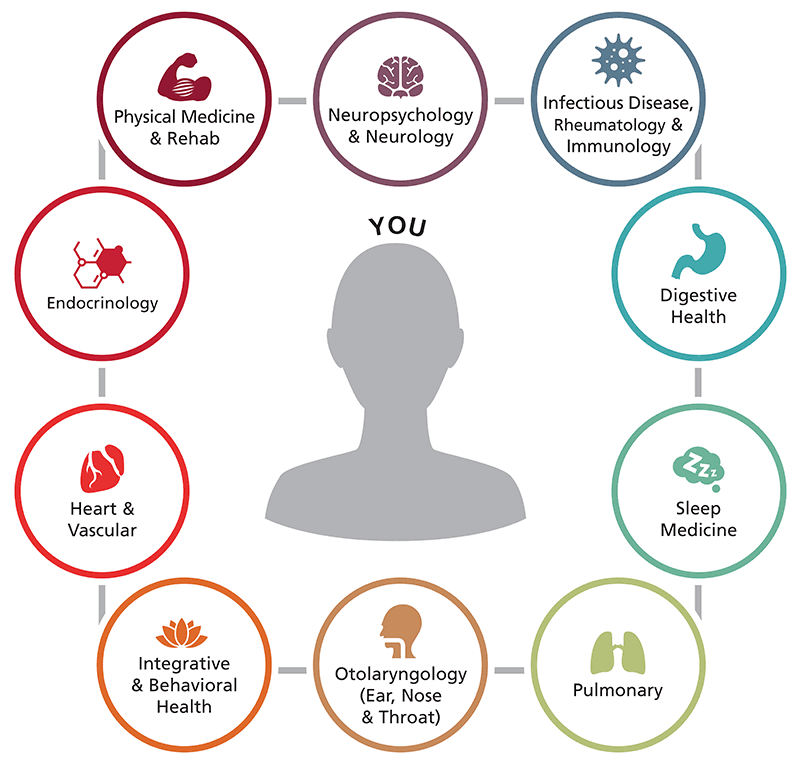
Integrated, Whole-Person Care
The UH COVID Recovery Clinic stresses the importance of treating the whole person. Whole-person care places an emphasis on integrative heath (stress management, relaxation techniques, acupuncture); behavioral health intervention for depression and anxiety or other psychological issues; rehabilitation services (PT, OT, neuropsychological rehabilitation); general pain management; and pulmonary/cardiac rehabilitation. In addition, we know that patients recovering from COVID often have sleep disturbances, which can lead to general symptoms of fatigue, weakness and cognitive impairment. Therefore, patients at the clinic will also be evaluated for sleep-related health issues and prescribed the appropriate therapies to improve their sleep.
The multidisciplinary team of COVID care providers described below will meet regularly to discuss cases. These discussions will help to ensure that the diagnostic and therapeutic approach to caring for each patient is optimized.
- Pulmonary
-
Respiratory complaints after acute COVID-19 often include, shortness of breath, chest pain and coughing. While generally such symptoms resolve over time, if they are persistent or are worsening they may indicate a given individual is developing a post-acute COVID respiratory complication, including pneumonia; worsening asthma; or blood clots within the lungs (pulmonary emboli).
The clinicians at the UH COVID Recovery Clinic will conduct a thorough assessment of each patient to determine how serious their condition is and create a customized treatment plan. Based on a given person's complaints the evaluation may include a chest X-ray, pulmonary functions tests, CT scan, echocardiography and even ultrasounds of the legs. If diagnostic testing is considered urgent it will be conducted the same day so results are available quickly and the appropriate treatment can begin.
In addition, it should be understood that shortness of breath is not always caused by respiratory dysfunction alone, but is often related to cardiac issues since the heart and lungs work in tandem. As a result, when evaluating shortness of breath in a patient recovering from COVID, cardiac testing is often needed as well.
Using a team-based, multidisciplinary approach, therapies for patients with respiratory symptoms may include:
- Treatments to manage worsening asthma or pneumonia
- Administration of blood thinners if blood clots are discovered within your lungs or legs (deep venous thrombosis)
- More advanced cardiac testing
- Cardiopulmonary Rehab - An exercise program to help patients expand their lungs more fully and improve shortness of breath
- Integrated Health - Holistic, supportive care to help patients manage the stress that can, in some cases, be the primary cause of their shortness of breath
- Heart & Vascular
-
Cardiac symptoms may include chest pain, irregular or rapid heartbeats, shortness of breath, dizziness and feeling faint. These symptoms can occur because COVID has caused damage to your heart muscle, blocked blood flow in your coronary arteries, caused inflammation of the lining around your heart or damaged the nerves that control your heart rhythm.
The clinicians at the UH COVID Recovery Clinic will conduct a thorough assessment of each patient to determine the severity of their condition. The evaluation will involve a variety of diagnostic tests which may include:
- Blood tests: To check for certain components in the blood that may indicate cardiac inflammation or other heart problems.
- Electrocardiogram (ECG): A noninvasive test that records the electrical activity of your heart. It can help detect abnormal heart rhythms.
- Echocardiogram: Uses ultrasound to check for any problems with your heart’s valves or chambers and measure how strongly your heart is pumping.
- Cardiac MRI: An imaging test that can detect inflammation of the heart muscle and lining around the heart and even heart blockages.
Using a team-based, multidisciplinary approach, the heart specialists at the UH COVID Recovery Clinic will devise a customized treatment plan for each patient with cardiac symptoms. Treatments may include medications and/or cardiopulmonary rehab to strengthen the heart muscle.
- Sleep Medicine
-
Sleep disturbances can lead to a dysfunctional sleep/wake cycle; worsening insomnia; new or worsening sleep apnea; daytime fatigue; weakness; excessive sleepiness; and even cognitive impairment. Those who had sleep problems like insomnia or sleep apnea before COVID may see worsening symptoms in the weeks and months that follow recovery. This may be due in part to the stress they experienced during their active treatment, particularly if it included hospitalization and/or intubation.
The sleep specialists at the UH COVID Recovery Clinic will evaluate those patients who report sleep-related health issues and prescribe the appropriate therapies to improve their sleep. These may include:
- A sleep study, which may be conducted in a UH sleep lab or at home.
- Sleep hygiene modifications like establishing routine bedtimes; eliminating or reducing the use of medications to induce sleep; and eliminating or reducing the use of stimulants like caffeine to counteract sleepiness.
- Lifestyle modifications such as reducing or eliminating screen time (TV and phone use) before bedtime
The UH COVID Recovery Clinic has a multidisciplinary sleep medicine group that includes specialists in neurology, psychiatry, family medicine and internal medicine who work together to devise the best treatment plan to restore and improve sleep for each patient. In addition, we collaborate with our colleagues in behavioral medicine and integrative health to provide patients with the tools to promote relaxation, manage stress and restore sleep health.
- Integrative & Behavioral Health
-
Behavioral health conditions in post-COVID patients may include heightened stress levels; new or worsening anxiety, depression or paranoia; and, in extreme cases, suicidal thoughts. In addition, patients hospitalized with COVID, particularly those requiring treatment in the intensive care unit, can have symptoms similar to Post Traumatic Stress Disorder (PTSD).
The clinical teams at the UH COVID Recovery Clinic are prepared to manage a broad range of behavioral health conditions and can assist with referrals to specialists as appropriate. We work together with neurology, sleep medicine, psychology, social work and the Connor Whole Health to provide patients with the best path forward to restore their mental health and get back to living the life they love. Treatments may include:
- Integrative health tools and interventions including stress management, relaxation techniques and acupuncture
- Medications to help stabilize new or worsening anxiety or depression
- Behavioral therapy and counseling to help patients understand what’s happening to them and teach coping mechanisms
- Neuropsychology & Neurology
-
In some people, their response to COVID-19 infection may include symptoms of confusion, memory loss, headache, dizziness, numbness, tingling and paralysis due to brain inflammation (encephalitis), stroke, neuropathy, spinal cord damage and damage to the autonomic nervous system. While neurologic complications of COVID occur more commonly in patients requiring hospitalization, related symptoms can persist and even newly develop during the recovery phase of COVID-19. In these situations, a comprehensive clinical assessment is necessary.
The clinical team at the UH COVID Recovery Clinic collaborates with neurologists and neuropsychologists to determine the best possible treatment plan for patients with neurological symptoms. Depending on the severity of their diagnosis, treatments may include:
- Medications to reduce inflammation and/or swelling
- Physical and/or cognitive rehabilitation
- Psychological evaluation and counseling
- Infectious Disease, Rheumatology & Immunology
-
Joint pain or swelling, fatigue, muscle pain and weakness, and new or ongoing chronic pain are symptoms that are often seen in the post-COVID patient. It is important that patients experiencing these symptoms be evaluated to determine if they are experiencing heightened inflammation related to COVID-19 or if an auto-immune disorder or infection is causing the problem.
For symptoms such as these, the clinical team at the UH COVID Recovery Clinic will collaborate with specialists in rheumatology, infectious disease and immunology to determine the root cause of the problem and devise an appropriate, multidisciplinary treatment plan. The first step will be to have the patient undergo a comprehensive physical exam that includes taking a complete medical history (pre- and post-COVID), blood tests and imaging exams. Depending on the findings of the exam, treatments may include:
- Anti-inflammatory medications to reduce swelling
- Antibiotic medications to treat infection
- Physical therapy
- Pain management
- Otolaryngology (Ear, Nose & Throat)
-
Persistent loss of taste and smell, sore throat, nasal congestion or drainage are the most common ENT symptoms reported by post-COVID patients. The wind pipe (trachea) may even be damaged during the acute course of COVID-19.
If a patient seen at the UH COVID Recovery Clinic reports symptoms related to the ear, nose and throat, such as those listed above, we will consult with a UH otolaryngologist and, when appropriate, refer the patient for specialized diagnosis and treatment.
- Digestive Health
-
Infection with COVID-19 can affect the GI tract by disrupting its functioning and reducing its ability to absorb fluids and electrolytes from the body. The liver, pancreas and gall bladder may also be damaged by the inflammation caused by COVID. Gastrointestinal symptoms may include appetite changes, upper abdominal pain, diarrhea, gastric reflux (acidity) and vomiting. Furthermore, elevated liver functions may be a sign liver damage.
If a patient seen in the UH COVID Recovery Clinic reports symptoms such as those described above, our team will conduct a thorough evaluation and make the appropriate referrals for specialty care. Digestive disorders such as these must be addressed quickly to avoid further complications such as bleeding in the GI tract. Recommended treatments may include:
- Medications to reduce acidity (i.e. proton pump inhibitors)
- Anti-nausea or anti-diarrheal medications
- Dietary and lifestyle modifications
- Endocrinology
-
Some patients may experience deficits of the endocrine system in the weeks and months after an acute COVID-19 infection. These may include new or worsening diabetes, thyroid damage and/or kidney damage leading to impaired renal function.
If a patient seen at the UH COVID Recovery Clinic reports any symptoms that indicate endocrine/metabolic dysfunction, such as those listed above, our team will conduct a thorough evaluation, which may include a physical exam, blood tests and imaging studies. When appropriate, we will consult with a UH endocrinologist and refer the patient for specialty care.
- Physical Medicine & Rehabilitation
-
Most patients will experience some degree of physical disability after an acute COVID-19 infection, particularly if they were hospitalized. This may be simply due to the deconditioning that results from having spent more time in bed, or it may be as a direct result of damage caused by the virus. Patients may have weakness in their legs, hands and fingers; generalized muscle pain; persistent fatigue; loss of physical endurance; and balance problems - all of which can lead to difficulties in performing the activities of daily living, and ultimately a loss of function and independence.
At the UH COVID Recovery Clinic, we have a team of physical medicine & rehabilitation specialists with the unique training and expertise to evaluate these symptoms in patients and, in collaboration with other team members, determine if they are caused by existing medical conditions like arthritis, or if they are COVID-related.
If symptoms are determined to be COVID-related, our physical and occupational therapists will work to create a customized exercise program for each patient, designed to improve their overall functioning and help them get back to their life and the activities they enjoy.
COVID Long-Haul Syndrome in Pediatric Patients
Although initial research suggests that fewer children than adults develop COVID Long-Haul Syndrome, there have been reported cases of persistent, often debilitating post-infection symptoms in pediatric patients. These may include diarrhea, extreme fatigue, stomach pain, new onset headache or migraine, and chronic, recurring fever.
The pediatric specialists at UH Rainbow Babies & Children’s Hospital have an assessment and treatment model for children that is similar to the adult COVID-19 Recovery Clinic.
If your child had COVID-19 and is now experiencing symptoms of COVID Long-Haul Syndrome, call 216-966-8000 to speak to our nurse navigator. Pediatric patients with suspected post-infection syndrome will be referred to Amy Edwards, MD, pediatric infectious disease specialist at UH Rainbow Babies & Children’s Hospital.
Contribute to COVID-19 Research
When you report and seek treatment for your COVID Long-Haul symptoms, not only are you getting the help you need to feel better, you are helping the medical community learn more about the long-term side effects of COVID-19. Over time, this will help doctors find more effective ways to detect and treat both acute COVID-19 infections and COVID Long-Haul Syndrome.
Participation is voluntary and all patient information is kept strictly confidential.
Schedule an Appointment
If, after your acute course of COVID-19, you are still experiencing symptoms, call us today to schedule an evaluation at
216-966-9000




