Hernia Surgery
Laparoscopic
What You Should Know:
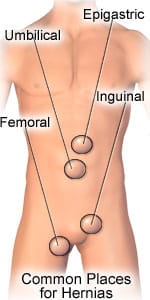
- Laparoscopic herniorrhaphy is surgery to repair a hernia. A hernia may occur when the muscle layers in your abdomen (stomach) weaken. The weakened muscle layers allow your tissues or organs to push through. When this happens, a bulge or mass (lump) may be seen or felt under your skin. Hernias often occur in your inguinal (groin) area. A hernia may also occur near your genital area (between your inner legs), or upper thigh. Hernias may also form in the front of your abdomen, or in areas of past surgical incisions (cuts).
- During this surgery, a special tool called a laparoscope is used. A laparoscope is a long metal tube with a light and camera on the end. The laparoscope will be inserted into your peritoneal cavity (the space in your abdomen containing organs). The laparoscope will allow your caregiver to see your hernia. You may have a hernia in one or both sides of your groin in need of repair. Laparoscopic surgery to fix your hernia may strengthen your abdominal muscles, remove your hernia bulge, and decrease your pain.
Care Agreement:
You have the right to help plan your care. To help with this plan, you must learn about your health condition and how it may be treated. You can then discuss treatment options with your caregivers. Work with them to decide what care may be used to treat you. You always have the right to refuse treatment.
Risks:
- You may be allergic to the anesthesia used during your surgery. You may also bleed more than expected during your surgery. During your surgery you may have injuries to your nerves, blood vessels or abdominal organs. The contents of your bowel may spill into your abdominal space and cause a very bad infection. In some cases, a TAPP hernia repair may need to be changed into an open hernia repair surgery. An open surgery means larger and deeper incisions will be made, which will take longer to heal. You may have shoulder and chest pain from the gas used during your surgery.
- You may have bruising, seroma (collection of fluid), swelling, or infection at your surgery site. After surgery, you may have trouble emptying your bladder. There is a risk of getting a blood clot in your leg or arm. This can cause pain and swelling, and it can stop blood from flowing where it needs to go in your body. The blood clot can break loose and travel to your lungs. A blood clot in your lungs can cause chest pain and trouble breathing. This problem can be life-threatening.
- You may have chronic (lasting) pain or numbness in your groin area for months or years after your surgery. You may need to have another surgery if your condition returns or occurs in a different area. If you do not have the surgery, your pain or discomfort may increase. Your soft tissue or bowels may become trapped in your abnormal opening. When tissues and organs are trapped they may become necrotic (tissue death). Trapped necrotic tissue and organs may be life-threatening. Talk to your caregiver if you have questions about your condition, surgery, or care.
Before Surgery
The week before your surgery:
- Make arrangements in advance for someone to drive you home from the hospital when it is time for you to leave. You cannot drive yourself home.
The day before your surgery:
- Our office will call you to give your surgery time and your arrival time.
Before your surgery:
- Informed consent: You have the right to understand your health condition in words that you know. You should be told what tests, treatments, or procedures may be done to treat your condition. Your doctor should also tell you about the risks and benefits of each treatment. You may be asked to sign a consent form that gives caregivers permission to do certain tests, treatments, or procedures. If you are unable to give your consent, someone who has permission can sign this form for you. A consent form is a legal piece of paper that tells exactly what will be done to you. Before giving your consent, make sure all your questions have been answered so that you understand what may happen.
During your surgery:
- You will be placed lying on your back with your feet slightly higher than your head. Your abdomen and groin area will be cleaned. Your caregiver will make 3 to 4 small incisions (cuts) around your groin area and into your peritoneal cavity. The laparoscope and other special surgery tools will be inserted through the incisions. Carbon dioxide gas may be used to inflate (make larger) your abdominal cavity. The gas will allow your caregiver to better see the area in need of repair.
- The weakened muscles in your groin will be checked through the scope. Your caregiver will remove your hernia or push it back into its normal space. A mesh patch will be placed over the area of the hernia and stapled or tacked in place. Your peritoneum (inner tissue lining of your abdomen) will then be closed over the mesh with staples or stitches. The carbon dioxide gas and surgery tools will be removed. Your incisions will be closed with stitches and covered with a bandage. The bandage will help keep your incisions clean and dry, and help to prevent infection.
After your surgery:
- You will be taken to a room where you will rest until you are fully awake. Once your caregivers see that you are okay, you may be able to go home. If your caregiver wants you to stay in the hospital, you will be taken to your room. Do not try to get out of bed until your caregiver says it is okay.
At home after surgery
Medicines:
- Keep a written list of the medicines you take, the amounts, and when and why you take them. Bring the list of your medicines or the pill bottles when you see your caregivers. Learn why you take each medicine. Ask your caregiver for information about your medicine. Do not use any medicines, over-the-counter drugs, vitamins, herbs, or food supplements without first talking to caregivers.
- Always take your medicine as directed by caregivers. Call your caregiver if you think your medicines are not helping or if you feel you are having side effects. Do not quit taking your medicines until you discuss it with your caregiver. If you are taking medicine that makes you drowsy, do not drive or use heavy equipment.
Follow-up visit information: Keep all of your planned visits with your caregiver. Write down any questions you may have. This way you will remember to ask these questions during your next visit.
Contact a Caregiver If:
- You are bleeding from your surgery site.
- You have a fever (high body temperature).
- Your have blood clots or fluid around your surgical site.
- Your surgery site is swollen, red, or has pus coming from it.
- You have chest pain or trouble breathing that is getting worse over time.
- You have questions or concerns about your medicine or care.
Seek immediate care if:
- You have pain in your surgery site that does not get better after taking pain medicine.
- You have trouble urinating.
- You notice a new hard lump at your surgery site.
- You suddenly have numbness in your groin area.
- You suddenly feel lightheaded and have trouble breathing.
- You have new and sudden chest pain. You may have more pain when you take deep breaths or cough. You may also cough up blood.
- Your arm or leg feels warm, tender, and painful. It may look swollen and red.


