Research Areas
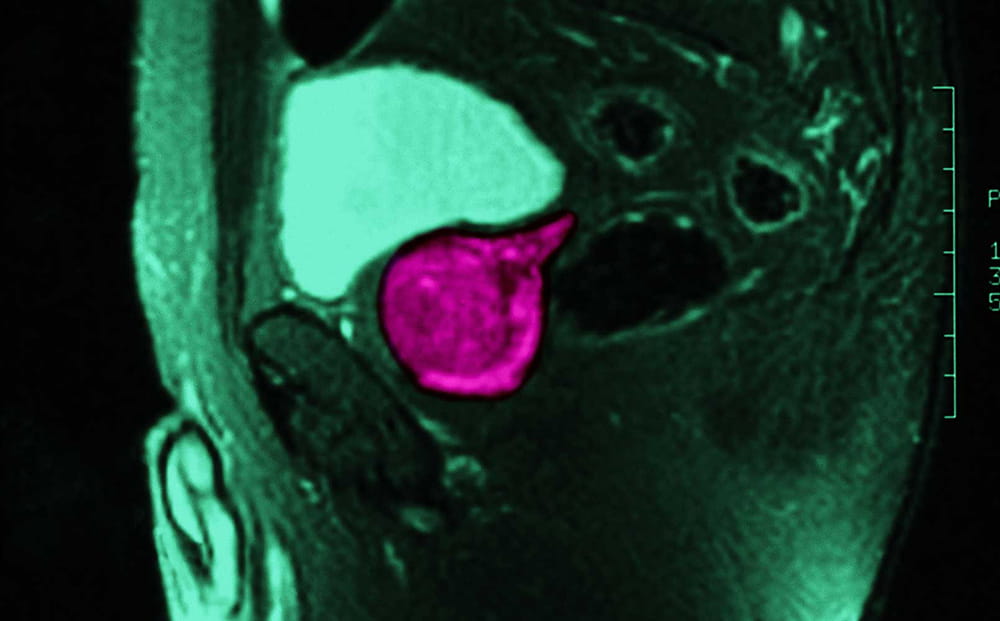
University Hospitals is dedicated to advancing men's health through faster, easier and more accurate prostate cancer diagnosis in hopes of reducing anxiety and creating a better experience overall.
Supported by a National Institutes of Health (NIH) grant, our team played an important role in a unique discovery that is now available to patients at University across Northeast Ohio. Dr. Lee Ponsky and his team developed a combined quantitative MRI and computerized decision support exam for more accurate detection and grading of prostate cancer both in the peripheral and transitional zones. It’s just one of the ways University Hospitals is researching, developing and delivering new and advanced patient care with these MRIs for prostate cancer screening.

Personalized Medicine Benefits Patients
A primary focus of the Urology Institute is to develop precision tools for cancer care. Jonathan Shoag, MD, a recent addition to the faculty, runs a translational research lab focused on bringing extensive data, genomic sequencing, and novel AI and statistical techniques to patients’ bedside. Recently, Dr. Shoag coauthored a Nature Communications publication illustrating how BPH, a very common disease of aging, has several different subtypes, which may be amenable to precision therapy.
An essential part of personalized medicine is understanding an individual patient’s risk. For example, prostate cancer is the second leading cause of cancer death in men in the U.S. In a recent New England Journal of Medicine article, Dr. Shoag illustrates that, over a man’s lifetime, using PSA to understand risk can have substantial benefits, which are likely more significant than the harms of screening.
Leveraging AI for Benign Urology
David Sheyn, MD is leveraging artificial intelligence (AI) to create complex prediction models to identify patients who respond to specific therapies for overactive bladders. Dr. Sheyn works with engineers at Case Western Reserve University to develop the AI algorithm for the management of the different conditions of overactive bladder. Dr. Sheyn’s recent research was published in the Journal of Obstetrics and Gynecology.
“Wouldn’t it be great to find a quicker resolution for these patients by predicting who might benefit from a particular medicine and who might fail and have to go on to next line therapy?”
- Britt Conroy, MD
Next Generation Biomaterial for Pelvic Reconstruction
Leading Edge Surgical Procedures and Research
Stress urinary incontinence (SUI) is involuntary leakage of urine due to weakening of pelvic muscles and ligaments which support the urethra. SUI occurs predominantly in the female population because of pregnancy and parity related trauma to the pelvic region. One in three women above the age 60 experience SUI. SUI is associated with a cost of tens of billions of dollars. Surgical treatment of SUI involve placement of a transvaginal sling. A sling is a tape-shaped biomaterial that supports and constricts the urethra to maintain continence. In 2012, 750,000 sling procedures/year were estimated in U.S. By 2020, number of procedures in the U.S is projected to reach 1,000,000/year. At the present, polypropylene slings are used as slings in majority of procedures with the rest being mostly limited to autografts.
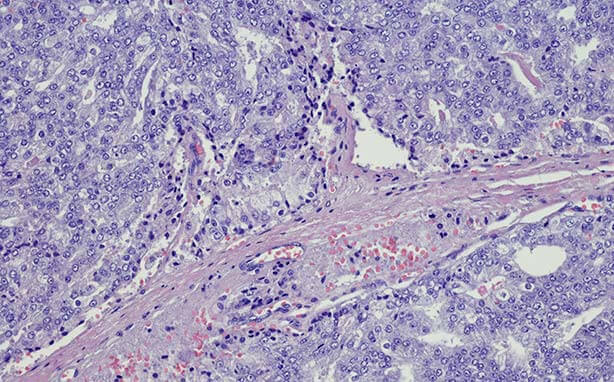
Drug Resistance Mechanisms in Prostate Cancer
Sanjay Gupta, PhD, professor, received $962,000 over three years from the Department of Defense to investigate drug resistance mechanisms in prostate cancer


