Septal Myectomy
What is septal myectomy?
Septal myectomy is a type of open-heart surgery for thick heart muscle (hypertrophic cardiomyopathy). It decreases symptoms of the condition.
A muscular wall called the septum separates the left and right ventricles, the 2 lower chambers of the heart. In hypertrophic cardiomyopathy, the walls of the ventricles and septum may thicken abnormally. The septum may bulge into the left ventricle and partially block the blood flow out to the body. This causes the heart to work harder. It also contributes to many symptoms of the disease, such as severe tiredness (fatigue) and shortness of breath.
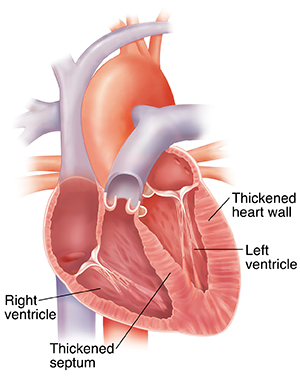
During septal myectomy, a surgeon removes excess muscle from the thickened septum. This lets the blood empty from the ventricle more easily.
Alcohol septal ablation is another option for treating cardiomyopathy. For this, the healthcare provider injects alcohol into a blood vessel in the ventricular septum. This causes some of the heart muscle cells to die, making the septum thinner. This treatment is not open-heart surgery, so recovery is much easier. But it may have an increased risk of certain complications, such as heart rhythm problems.
Why might I need septal myectomy?
In many cases, medicines are enough to relieve symptoms of hypertrophic cardiomyopathy. If symptoms are not relieved with medicines, a procedure such as septal myectomy is often effective.
Septal myectomy is a relatively safe surgical procedure that surgeons have done for many years. Some people with hypertrophic cardiomyopathy also might need a septal myectomy before becoming pregnant, even if their symptoms aren’t severe.
Talk with your healthcare provider to find out if you are a good candidate for either septal myectomy or alcohol septal ablation. Review the risks and benefits of each procedure with your provider. Surgery is often preferable in younger people and in people with more severe thickening. You might have septal anatomy that is better suited to surgery. You might need more work done on the heart, like repair of the mitral valve. In these cases, septal myectomy is preferable.
What are the risks of septal myectomy?
The risks of complications from septal myectomy are low, but they do sometimes happen. Your own risks will vary based on your age and other factors. Talk with your healthcare provider about any concerns you may have. Some possible complications include:
- Irregular heart rhythms, such as heart block. You may need a pacemaker.
- Infection
- Bleeding
- Cardiac tamponade
- Blood clots leading to stroke or heart attack
- Complications from anesthesia
- Need for more surgery. The condition may come back, or you may need to have more heart muscle removed.
- Removal of too much heart muscle. This can cause a ventricular septal defect (VSD).
- Blood flow problems during surgery that can lead to poor pumping function of the heart in the future
- Death
Heart block is one of the more common complications. Heart block is a disruption to the electrical signals through the heart. This can cause your heart to beat too slowly. Certain kinds of heart block require treatment with a pacemaker.
Certain factors increase the risk of complications. Some of these are as follows:
- Chronic illness
- Other heart conditions
- Lung problems
- Increased age
- Being obese
- Being a smoker
- Infections
- Diabetes
How do I get ready for septal myectomy?
Talk with your healthcare provider about how to prepare for your upcoming surgery. Remember the following:
- Follow all directions you are given for not eating or drinking before surgery.
- Try to stop smoking before your procedure. Ask your provider for help.
- You may need to stop taking certain medicines before your surgery. Follow your provider’s instructions if you normally take blood-thinning medicines such as warfarin or aspirin.
You may need to arrive at the hospital the afternoon before your procedure. You will be asked to sign a form consenting to the surgery. This is a good time to ask any questions you have about the procedure. You may need some routine tests before the procedure to assess your health before surgery. These may include:
- Chest X-ray
- Electrocardiogram (ECG)
- Blood tests
- Echocardiogram
- Cardiac catheterization
If needed, someone will shave your skin above the surgical area. About 1 hour before the procedure, you will be given medicines to help you relax. In most cases, your surgery will proceed as planned. But sometimes another emergency might delay it.
What happens during septal myectomy?
Check with your healthcare provider about the details of your procedure. In general, during your septal myectomy:
- A provider will give you anesthesia before the surgery starts. This will cause you to sleep deeply and painlessly during the procedure. Afterward, you won’t remember it.
- The surgery will take several hours. Family and friends should stay in the waiting room so the surgeon can update them.
- Your surgeon will make a cut (incision) down the middle of your chest and separate part of your breastbone.
- The surgery team will attach you to a heart-lung machine. This machine will provide oxygen to your blood and pump the blood to your body during your surgery.
- Your surgeon will remove part of your thickened septum
- The surgery team will remove the heart-lung machine.
- The team will wire your breastbone back together.
- The team will then sew or staple the incision in your skin back together.
What happens after septal myectomy?
In the hospital
- When you wake up, you might feel confused at first. You might wake up a couple of hours after the surgery, or a little later.
- The team will carefully watch your vital signs, such as your heart rate. They may hook you up to a few machines so the nurses can check these more easily.
- You may have a tube in your throat to help you breathe. This may be uncomfortable, and you won’t be able to talk. Someone will often remove the tube within 24 hours.
- You may have a chest tube to drain excess fluid from your chest.
- Bandages will cover your incision. These often can come off in a few days.
- You will feel some soreness, but you shouldn’t feel severe pain. If you need it, you can ask for pain medicine.
- In 1 or 2 days, you should be able to sit in a chair and walk with help.
- You may do breathing therapy to help remove fluids that collect in your lungs during surgery.
- You will likely be able to drink liquids the day after surgery. You can have regular foods as soon as you can tolerate them.
- You may get elastic stockings to help blood circulate through your leg veins.
- You will likely need to stay in the hospital around 5 days.
At home
- Make sure you have someone to drive you home from the hospital. You will also need some help at home for a while.
- You will likely have your stitches or staples removed in a follow-up appointment in 7 to 10 days. Be sure to keep all follow-up appointments.
- You may tire easily after the surgery. But you will slowly start to recover your strength. Recovery time varies, but it will be at least a few weeks.
- After you go home, take your temperature and your weight every day. Call your healthcare provider right away if your temperature is over 100.4°F (38˚C), or if your weight changes.
- Ask your provider when it is safe for you to drive.
- Don't lift anything heavy for a few weeks. Ask your provider about what is safe for you to lift.
- Follow all instructions your provider gives you for medicines, exercise, diet, and wound care.
Next steps
Before you agree to the test or the procedure, make sure you know:
- The name of the test or procedure
- The reason you are having the test or procedure
- What results to expect and what they mean
- The risks and benefits of the test or procedure
- What the possible side effects or complications are
- When and where you are to have the test or procedure
- Who will do the test or procedure and what that person’s qualifications are
- What would happen if you did not have the test or procedure
- Any alternative tests or procedures to think about
- When and how you will get the results
- Who to call after the test or procedure if you have questions or problems
- How much you will have to pay for the test or procedure


