Superior Outcomes in Lung Surgery
UH Cleveland Medical Center has outcomes near the top 10 percent of all major academic medical centers for lung resection, as assessed by the Society of Thoracic Surgery National Database. The division also has consistently shorter length of stay and lower perioperative mortality for major lung procedures than most tertiary academic medical centers.
Quick Facts
Expertise for the High-Risk Patient
UH Cleveland Medical Center is recognized as a center of excellence in high-risk lung surgery. It has specialized expertise in treating the elderly, patients with severe emphysema, and those deemed too high-risk for traditional surgical methods. For patients deemed too high-risk for minimally invasive, limited resection, then noninvasive techniques such as stereotactic body radiation, microwave ablation or cryotherapy are available.
Robotic Thoracic Surgery
Robotic surgery uses small incisions similar to those used during video-assisted thoracic surgery (VATS). Instead of doing the procedure at the operating room table, a UH surgeon is seated at the robot console and remotely controls robotic arms that operate. The robotic camera allows for 3-D visualization, and the robotic arms allow for fine movements in tight spaces such as the center of the chest. Length of stay, complication, and cure rates are similar to that seen with VATS.
Video-Assisted Thoracic Surgery (VATS)
VATS is a minimally invasive alternative for the diagnosis and treatment of patients with lung cancer. VATS involves smaller incisions with no large muscle division, no rib division, and no rib spreading. With oncological results identical to those seen when using the open technique, patients benefit from less postoperative pain, fewer complications, lower transfusion requirements, less tissue loss and scarring, and faster return to normal activities.
This novel technique is used at UH Cleveland Medical Center in 94 percent of all lobectomies for stage I lung cancer, higher than the average 74 percent use rate at other tertiary care hospitals. It is also routinely used for smaller lung resections, pleural procedures (effusions), mediastinal surgery, and esophageal surgery.
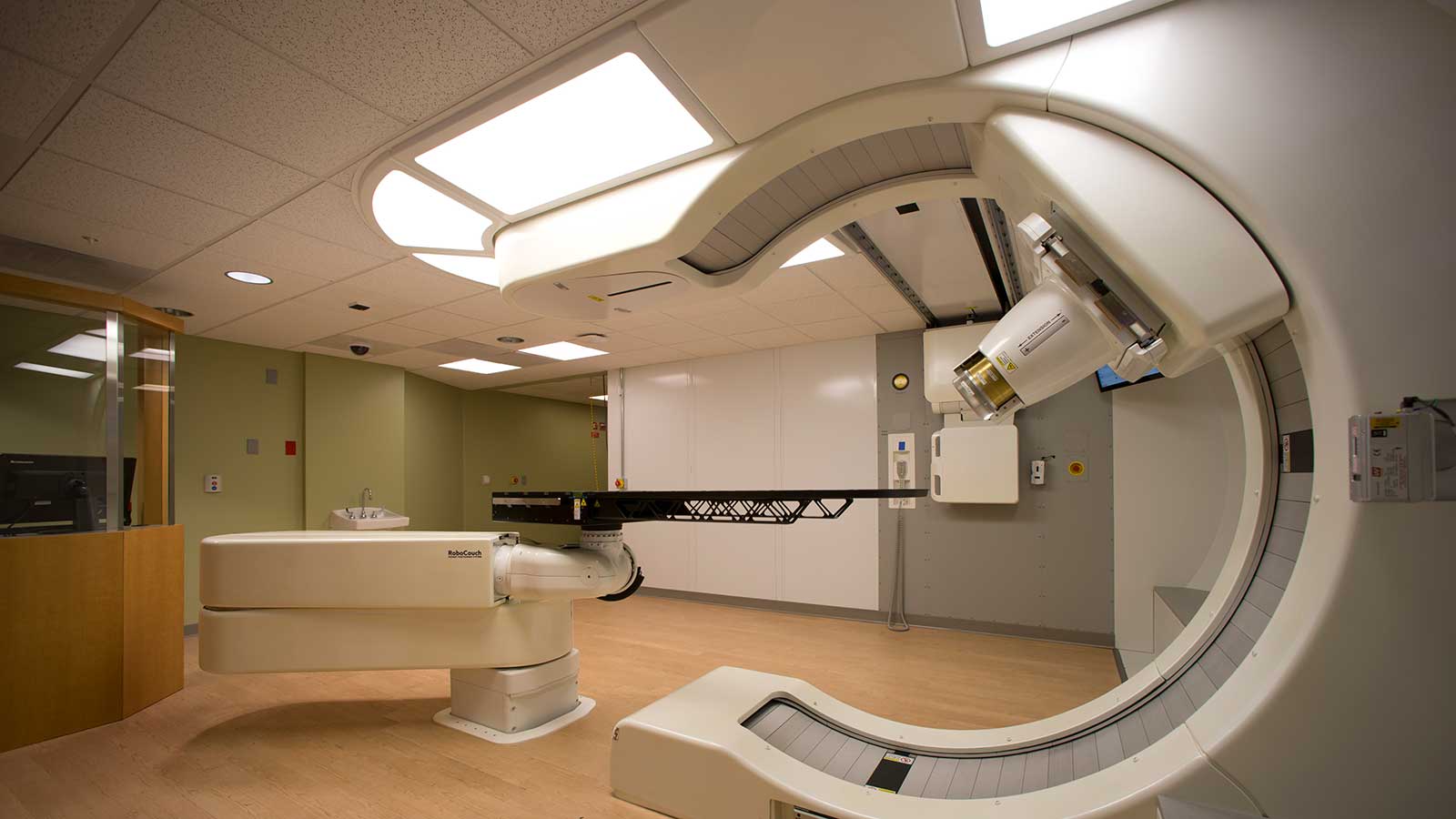
Proton Therapy for Thoracic Malignancies
Proton Therapy, such as provided at the UH Proton Therapy Center, is uniquely suited for treating the tumors of the chest. This targeted therapy allows for potentially curative radiation doses to be administered to tumors near the heart and spinal cord while sparing those vital structures from potentially damaging radiation.
Similar to conventional high energy X-rays, proton therapy is an external beam radiation therapy technique. The difference is that protons are larger and heavier charged particles that deposit the radiation dose in a more targeted manner. By changing the proton beam's energy, radiation oncologists can tailor the proton dose to the specific depth and shape of the tumor, while significantly reducing the dose to surrounding healthy tissue.
When used in the treatment of specific tumors, proton therapy can decrease side effects, resulting in a better quality of life during treatment and the potential to reduce the risk of developing radiation-induced secondary cancers decades after treatment.
This leading-edge technology further enhances the advanced treatment options available through University Hospitals Seidman Cancer Center.
UH has the only proton center in Northern Ohio.


