Nosebleed (Epistaxis) in Children
What is a nosebleed in children?
A nosebleed is bleeding from tissues inside the nose (nasal mucus membranes) caused by a broken blood vessel. The medical word for nosebleed is epistaxis. Most nosebleeds in children occur in the front (anterior) part of the nose close to the nostrils. This part of the nose has many tiny blood vessels. These can be damaged easily. These nosebleeds are usually not serious.
Nosebleeds in the back part of the nose, near the throat (posterior) are less common in children than nosebleeds in the front. They can be more serious and cause a lot of blood loss.
A nosebleed can look scary, but is usually not a serious problem. Nosebleeds are common in children. They happen more often in dry climates. They also happen more during the winter. That’s when dry heat in homes and buildings can cause drying, cracking, and crusting inside the nose. Many children outgrow nosebleeds during their teen years.
What causes a nosebleed in a child?
Nosebleeds can be caused by many things. Some common causes include:
- Dry air
- Picking the nose
- Blowing the nose too hard
- Injury to the nose
- Colds and allergies
- Objects in the nose
- Medicine
In many cases, no specific cause for a nosebleed is found.
Which children are at risk for a nosebleed?
A child may be more at risk for nosebleed if they:
- Live in a dry climate
- Pick their nose
- Has allergies
- Has a cold
What are the symptoms of a nosebleed in a child?
The main symptom of a nosebleed is blood dripping or running from the nose. Bleeding from the mucus membranes in the front part (anterior) of the nose comes from only one nostril. Bleeding higher up in the nasal cavity may come from both nostrils. It may be painless. Or your child may have pain caused by an injury or an area of sore tissue inside the nose.
The symptoms of a nosebleed can be like other health conditions. Make sure your child sees their healthcare provider for a diagnosis.
How is a nosebleed diagnosed in a child?
The healthcare provider will ask about your child’s symptoms and health history. They may also ask about any recent accidents or injuries. They will give your child a physical exam.
How is a nosebleed treated in a child?
- Keep your child calm and comfort them. Tell your child to breathe normally out of their mouth.
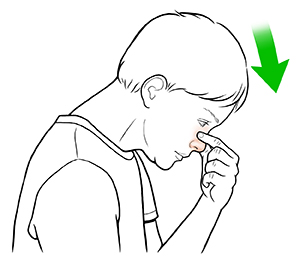
- Have your child stand or sit up and lean their head forward to help stop them from swallowing the blood. This also prevents the blood from pooling in the throat. Keep a cloth or towel under their nose to absorb any blood. Don't have your child lie down or tilt their head back. If your child appears to be swallowing blood or has a lot of blood in the mouth, have them spit the blood out. If blood is swallowed, it can lead to vomiting.
- Don’t have your child put their head between the knees. This can make bleeding worse.
- Don’t put tissues or gauze in your child’s nose.
- Have your child gently blow their nose. Then squeeze the lower third (the soft part, not the bridge of the nose) of the nose with your thumb and forefinger. Younger children may not understand how to gently blow their nose.
- Continue squeezing your child's nose closed for 5 to 10 minutes. Don’t stop pinching to check if bleeding has stopped.
- If bleeding continues, repeat the step above by squeezing the nose for 5 to 10 minutes without looking to see if bleeding has stopped.
- You may also put a cold compress on the bony bridge of the nose. Wrap cold compresses in a thin towel. Do not put them directly on the skin.
- Once the bleeding stops, tell your child not to rub, pick, or blow their nose for 2 to 3 days. This will let the broken blood vessel heal.
- If the bleeding doesn’t stop, contact your child's healthcare provider right away or go to the emergency room or urgent care clinic.
If your child’s nose doesn’t stop bleeding, take them to see the healthcare provider or go to the emergency room. In some cases, a provider may apply a chemical or heat to close a blood vessel. This is called cauterization. The provider may pack the nose as another option. Both are quick procedures. Talk with your child’s healthcare providers about the risks, benefits, and possible side effects of all treatments.
How can I help prevent a nosebleed in my child?
If your child has nosebleeds often, you can help prevent them in these ways:
- Treating nasal allergies may help stop cycles of itching, picking or scratching, and bleeding. Talk with your child's healthcare provider if your child has allergies that often lead to nosebleeds. Contact your child's healthcare provider before giving them any over-the-counter medicine, especially for the first time.
- Run a cool mist humidifier in your child's room at night, if the air in your home is dry. Clean the humidifier regularly so germs and mold don’t grow in it.
- Teach your child not to pick their nose or blow it too hard. Nose picking is a common cause of nosebleeds.
- Teach your child not to stick foreign objects in their nose.
- Your child's healthcare provider may advise you to use a nasal saline spray, nasal gel, or nasal ointment to moisten the inside of your child's nose. This is often done in the winter. Follow all directions when using these on your child. This treatment also helps protect the mucus membranes in the nose.
- Use saltwater (saline) nose drops or spray as directed by your child's healthcare provider.
- Don’t smoke or allow others to smoke in the home or around your child.
- Never give your child or teen aspirin. It could cause a rare but serious condition called Reye syndrome.
Important
Based on the age of your child, the cause of their nose bleed, or both, your child's healthcare provider will tell you the correct way to care for your child's nosebleed. Always contact your healthcare provider to discuss your child's nosebleeds.
Key points about a nosebleed in children
- A nosebleed is bleeding from tissues inside the nose (nasal mucus membranes) caused by a broken blood vessel.
- A nosebleed can look scary, but is usually not a serious problem. Nosebleeds are common in children. They happen more often in dry climates. They also happen more during the winter. That’s when dry heat in homes and buildings can cause drying, cracking, and crusting inside the nose.
- Nosebleeds can be caused by many things, such as dry air, nose picking, injury, medicines, and allergies. In many cases, no specific cause for a nosebleed is found.
- Have your child sit up and lean forward. Don’t have your child lie down or lean their head back. This is to prevent them from swallowing blood. Swallowing blood may make your child vomit.
- Squeeze the nostrils closed for 5 to 10 minutes. Don’t stop pinching to check if bleeding has stopped.
- Run a cool mist humidifier in your child's room at night, if the air in your home is dry. Teach your child not to pick their nose or blow it too hard. Your child's healthcare provider may advise you to use a nasal saline spray, nasal gel, or nasal ointment, especially in the winter, to moisten the inside of your child's nose. Follow all directions when using these on your child.
Next steps
Tips to help you get the most from a visit to your child’s healthcare provider:
- Know the reason for the visit and what you want to happen.
- Before your visit, write down questions you want answered.
- At the visit, write down the name of a new diagnosis, and any new medicines, treatments, or tests. Also write down any new directions your provider gives you for your child.
- Know why a new medicine or treatment is prescribed and how it will help your child. Also know what the side effects are.
- Ask if your child’s condition can be treated in other ways.
- Know why a test or procedure is recommended and what the results could mean.
- Know what to expect if your child does not take the medicine or have the test or procedure.
- If your child has a follow-up appointment, write down the date, time, and purpose for that visit.
- Know how you can contact your child’s healthcare provider after office hours, and on weekends and holidays. This is important if your child becomes ill and you have questions or need advice.


