Facial Reanimation Surgical Procedures
If conservative treatments like medications and physical therapy fail to restore function and/or symmetry in patients with facial paralysis, surgery may be a treatment option.
Facial reanimation procedures are extremely intricate surgeries given the proximity of the facial nerve to other important structures, including the eighth cranial nerve which is responsible for hearing and balance. The ENT facial plastic surgeons at University Hospitals have the advanced training, skills and experience to perform these delicate procedures and provide their patients with the best possible cosmetic and functional outcomes.
Your health is important. Get expert care.
If your facial paralysis symptoms persist and do not improve with conservative treatments, call 216-844-3223 to schedule an in-person consultation with a UH ENT facial plastic surgeon.
Virtual appointments are also available.
A Comprehensive Evaluation Is the First Step
Our surgeons will first perform an in-depth consultation to assess the patient’s facial nerve and muscle function, facial symmetry and any related speech, breathing or eating problems. They will also take a medical history and make note of which treatments and therapies have already been tried. They will then offer recommendations for surgical procedures that may relieve the patient’s symptoms, restore function and/or improve appearance. All procedures are performed through incisions that are aesthetically hidden for an optimal cosmetic outcome.
Surgical Treatment Options
Surgical options for the treatment of facial paralysis will be determined by how long the patient has been experiencing symptoms, the severity of the paralysis and the specific facial organs affected. Based on the results of the comprehensive evaluation, your surgeon may recommend one or more surgical procedures. These may include:
Eyelid Closure
Facial paralysis that prevents the eye(s) from fully closing can put the eye at risk for excessive dryness and loss of sensation, which can ultimately lead to eye ulceration and infection. If nonsurgical treatments such as eye lubrication and external eyelid weights are not sufficient, we offer a surgical procedure to correct eyelid closure. During the surgery, we place a thin platinum weight under the upper eyelid skin to help achieve better descent of the eyelid and full eyelid closure. The weight can be removed at any point if it is determined it is no longer required.
Facial Nerve Decompression
When the facial nerve is compressed by surrounding bone or muscle due to injury or disease, the associated facial muscles can become numb or paralyzed. Decompression surgery removes whatever is pressing on the nerve to relieve the pressure, improve blood circulation and restore feeling and function. Nerve decompression surgery is most effective for acute episodes of facial paralysis in which symptoms have been present for less than three weeks.
Facial Nerve Repair and Grafting
If the facial nerve itself is diseased or damaged, a direct nerve repair may be a good surgical option. In this procedure, the affected segment of the nerve is removed and the two nerve ends reconnected. If there is not a sufficient length of nerve to reconnect the ends, a piece of nerve taken from elsewhere in the body may be used to “bridge” the gap created once the injured portion is removed. This is called a nerve graft.
Selective Myectomy
Muscle myectomy is a surgery involving removal of a muscle that is moving unfavorably, commonly seen in patients who experience a limited recovery after facial paralysis. The most common reason for this procedure is to treat muscles around the mouth or neck that are pulling the corner of the lip down, leading to discomfort or an abnormal smile. A myectomy can remedy this by removing a portion of the dysfunctional muscle. Often, we would first inject Botox® into these muscles to temporarily weaken them and investigate if a myectomy would be effective as a long-term option.
Facial Nerve Transfer and Reinnervation
If the original source of input into the facial nerve and muscles is limited or completely unavailable and we know the facial nerve will not regenerate, a nerve transfer procedure may be recommended. In these procedures, a nearby, healthy nerve or nerve branch is cut and its end is sutured to the non-functioning nerve. Over time, the healthy nerve will grow into the damaged one and restore movement to the associated muscle(s). There are three main nerve transfer procedures that may be performed alone or in combination with one another. These include:
Cross Face
Nerve Graft
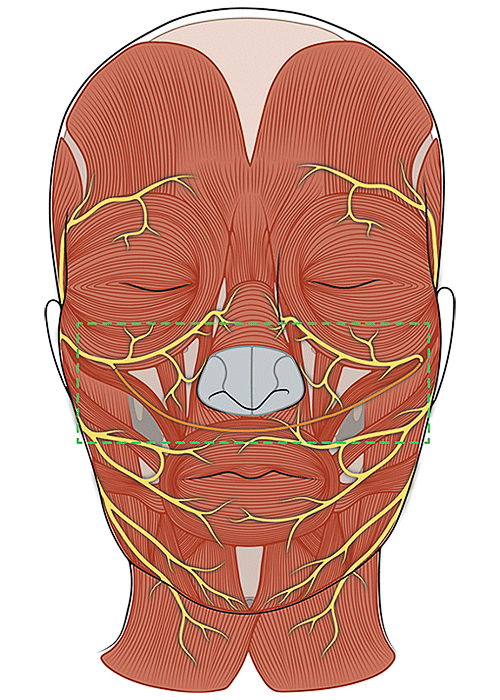
This procedure involves taking a sensory nerve from the neck, arm or leg and attaching it to a facial nerve branch on the non-paralyzed side of the face, tunneling it across the face and connecting it to nerves on the paralyzed side to restore function.
Masseter Nerve
Transfer
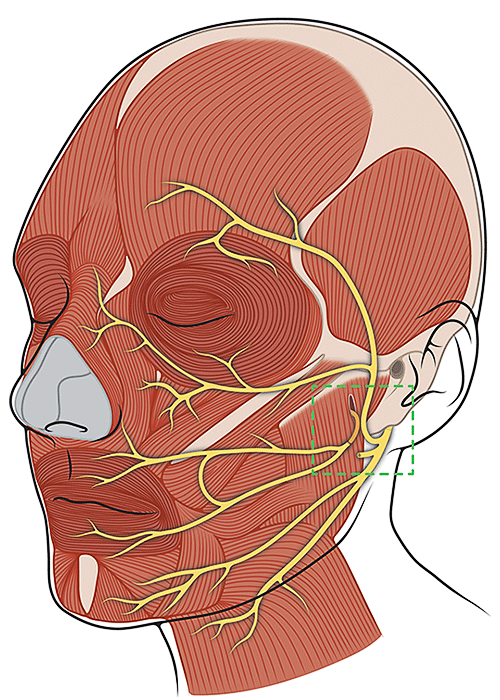
This procedure involves dividing the masseteric nerve (which runs through the muscle we use for chewing) and connecting one end to a branch of the facial nerve. This procedure is a reliable way to restore movement of the lip and cheek on the paralyzed side.
Hypoglossal Nerve Transfer
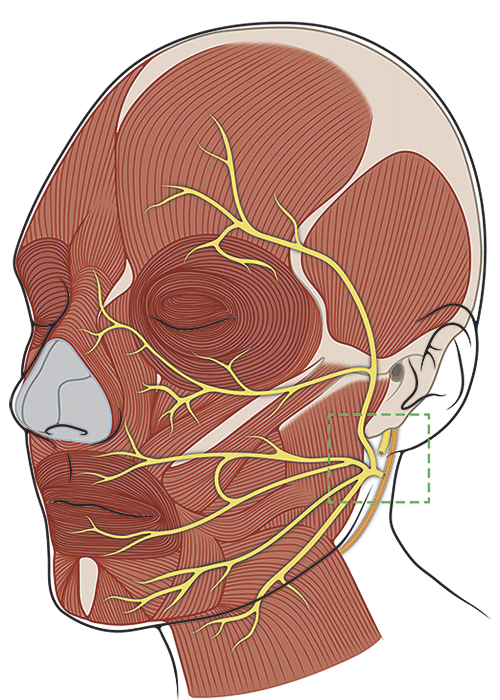
This procedure involves dividing the hypoglossal nerve (which controls tongue movement) and attaching one end to the facial nerve to improve facial tone and symmetry. There is some risk of tongue weakness following this procedure but this can often be resolved with appropriate therapies.
Muscle Transfer
Long-term facial paralysis (more than two years) often leads to atrophy of the facial muscles which have lost function. In these cases, the muscles usually cannot be reanimated even if the facial nerve is the body, “transplanting” them in the face and reanimating them by connecting them to the facial nerve. Muscle transfers may require more than one procedure and several brief hospital stays. Procedures may include:
Temporalis Tendon Transfer
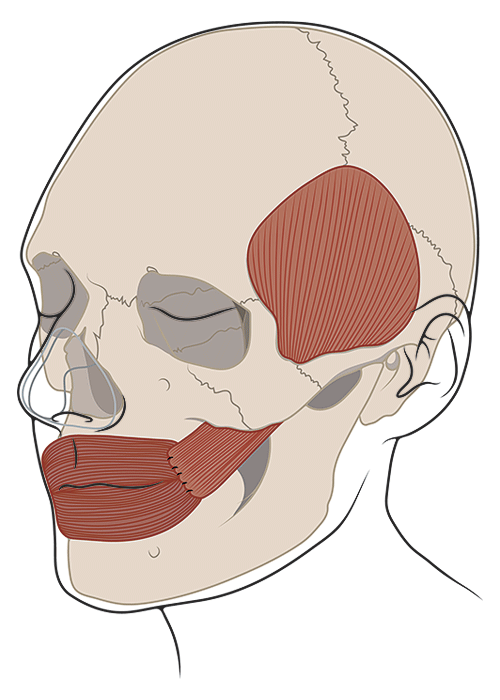
The temporalis muscle lays over the side of the skull and attaches to the jaw to help close the mouth and clench your teeth together. We can provide movement to the corner of the mouth by detaching this muscle from the jaw and re-attaching it to the lip. The beauty of this procedure is it can be hidden either through an incision in a crease on the cheek or in the mouth. Once it has healed, the lips will be in better position and the corner of the mouth will move up with clenching (similar to a sile). We usually overcorrect the smile at first because over time this muscle relaxes to provide great symmetry. As one can imagine, clenching your teeth is how you would control the muscle and that means the patient needs retraining and rehabilitation to get the best outcome from surgery.
Gracilis Muscle
Transfer
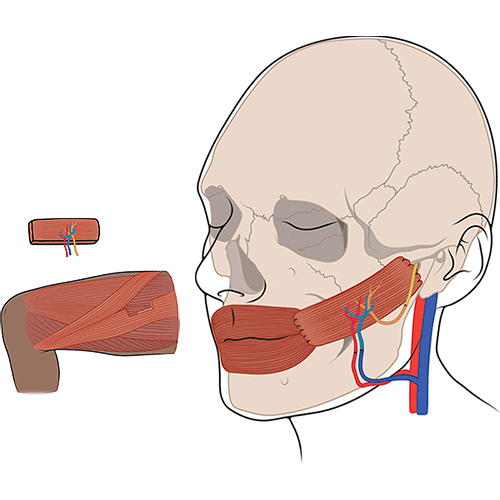
The gracilis free flap takes a muscle from the leg and transfers it to the face. We reattach both blood and nerve supplies to achieve healthy and desirable movement. This procedure often involves two stages of surgery separated by 6 – 8 months. We perform these surgeries through incisions hidden along the hairline and around the ear similar to a facelift surgery. The first stage of surgery takes a nerve from the side of the leg to attach to a facial nerve on non-paralyzed side of the face. We tunnel this nerve across the face to be primed for the next stage of surgery that is the muscle transfer. For the second surgery, we attach the gracilis muscle to the previously tunneled nerve, as well as a second nerve we use to chew (the masseteric nerve). This provides the mouth muscle with coordinated and strong movement, leading to more facial symmetry. The muscle takes up to 6 months to begin moving and continues to improve with retraining and rehabilitation over the next few years.
Selective Neurectomy
Abnormal, uncoordinated muscle movements of the face (synkinesis) is often due to abnormal nerve activity in patients who experience a limited recovery after facial palsy. Neurectomy is a procedure during which we excise the specific nerves that are no longer communicating properly with the facial muscles The malfunctioning nerves are identified and either cut out or rerouted to improve facial movement. Similar to myectomy, we will often try Botox® injections first to ensure a neurectomy is necessary for an optimal outcome.
Your health is important. Get expert care.
If your facial paralysis symptoms persist and do not improve with conservative treatments, call 216-844-3223 to schedule an in-person consultation with a UH ENT facial plastic surgeon.
Virtual appointments are also available.


