New Imaging Techniques to Identify Coronary Disease
June 09, 2019
Can a common chest x-ray help detect heart disease?
Innovations in Cardiovascular Medicine & Surgery - Summer | 2019
It’s estimated that clinicians generate more than 450 million chest x-rays each year worldwide, making it the world’s most common imaging procedure. A team at University Hospitals and Case Western Reserve University wants to put these x-rays to work to aid with early diagnosis of coronary artery disease and valvular heart disease.
The x-ray that could accomplish this is a dual-energy chest x-ray.
“Usually when you do a standard chest x-ray, a single energy beam passes through the patient,” says Robert “Chip” Gilkeson, MD, Division Chief of Cardiothoracic Imaging at UH Cleveland Medical Center and Director of the Cardiovascular Imaging Center of UH Harrington Heart & Vascular Institute; and Professor of Radiology, Case Western Reserve University School of Medicine. “But dual energy technology has a way to send two different x-ray beams of different energies. Through a lot of complicated physics, you can highlight and visualize certain tissues. Using the digital subtraction, material decomposition technique, a bone/calcium image can be computed which suppresses the soft tissue component.”
 Robert "Chip" Gilkeson, MD
Robert "Chip" Gilkeson, MDDr. Gilkeson and his colleagues began experimenting with this technique several years ago to help identify coronary calcium. The team includes biomedical engineer David L Wilson, PhD, Professor of Biomedical Engineering from Case Western Reserve University, as well as collaborators from University Hospitals: Alan Markowitz, MD; Joseph Sabik, MD; Sanjay Rajagopalan, MD; Marco Costa, MD, PhD, MBA; Guilherme Attizzani, MD; Philipp Graner; Lisa Youngblood; Jennifer Sposato; Victoria Uram and Leslie Ciancibello.
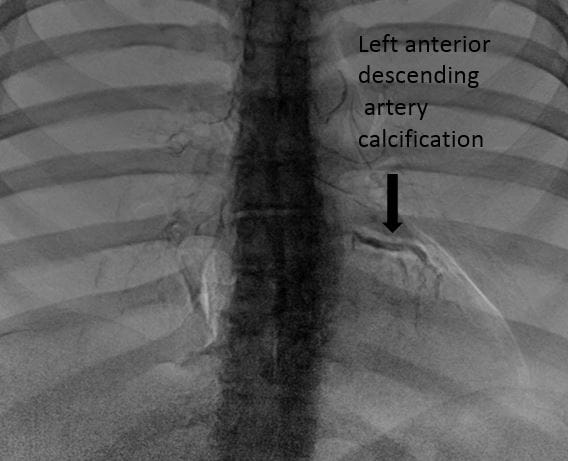
“Through a series of studies, we looked at calcified structures that we thought were corresponding to the coronary arteries,” Dr. Gilkeson says. “In patients who had a dedicated angiogram or a CT scan, we confirmed that the calcifications we were seeing on x-ray were indeed true calcifications in the coronary arteries.”
This led Dr. Gilkeson and his colleagues to wonder whether a dual-energy chest x-ray might be an alternative to traditional CT coronary calcium scoring – with clear advantages in safety and cost.
“A lot of our studies have shown that in the right population, we can almost develop a calcium score for an x-ray,” he says. “That could be potentially very helpful as a screening tool. We do a lot of CT for calcium scoring, but a lot of places in the world don’t do that. The radiation dose is very low on a CT scan, but for a chest x-ray, the radiation dose is less than 10 percent of that. Also, in general, an x-ray is much less expensive than a CT scan. So we thought this might be a lower risk, lower cost way to see coronary calcium.”
“We’re always working to find affordable solutions for cardiovascular disease screening that can be easily implemented in the community,” says Marco A. Costa, MD, PhD, MBA, President of the UH Harrington Heart & Vascular Institute. “Dual-energy x-ray technology can help us achieve that important vision. It very well could be part of defining the future of cardiovascular medicine.”
Dr. Gilkeson and his colleagues are next applying this idea to patients with aortic stenosis – a growing problem in an aging population.
“Can we visualize aortic valve calcification or aortic stenosis on a dual energy x-ray?” he asks. “We officially had our first patient yesterday to try to find out. We’re looking to provide proof of concept, so we will be looking at our TAVI patients who we know have calcium on their CT scans just to see if we can visualize that calcium on a dual energy x-ray.”
The team is also working to develop software called CorCalDx, with funding from the Coulter Foundation. Once complete, this software will enable fast and high throughput detection of coronary calcium using the commonly ordered dual-energy chest x-ray.
In addition, work is under way to develop an artificial intelligence tool that would be able to recognize coronary calcium on dual-energy chest x-rays. This would allow for standardized, highly reliable readings, while reducing the burden on clinicians.
In the end, Dr. Gilkeson believes this work could have major implications for early detection of heart disease.
“We know that people have chest x-rays for a lot of different reasons – before surgery, maybe for pneumonia, and we know that coronary artery disease and aortic stenosis many times goes underdiagnosed until people get really symptomatic,” he says. “Maybe the dual-energy chest x-ray would be a nice screening or at least early detection tool to alert the clinician that his or her patient may have significant coronary artery disease or even valve disease.”
Within the UH system, dual-energy x-rays are available at UH Cleveland Medical Center, UH Mentor Hopkins Health Center, UH Twinsburg Health Center, UH Minoff Health Center at Chagrin Highlands, UH Broadview Heights Health Center, as well as UH Hudson Health Center.
For more information about this work, please email Robert.Gilkeson@UHhospitals.org.


