Varicose and Spider Veins: What's the Difference – and What To Do
September 20, 2021
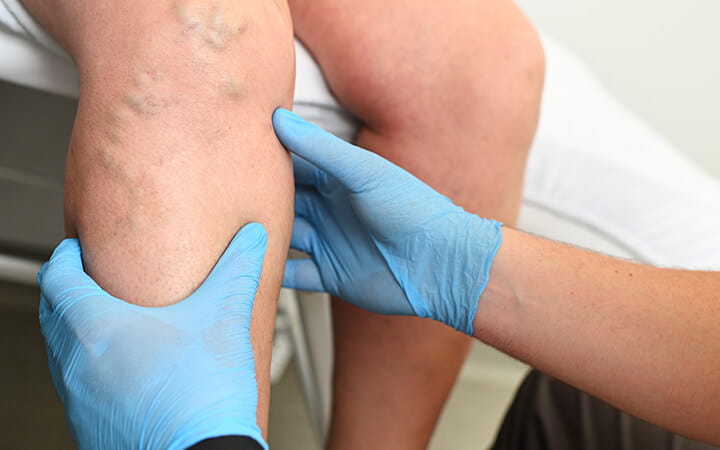
Varicose and spider veins affect men as well as women and impact the quality of life for a large segment of the population.
Excess weight, age, family history, pregnancy, hormonal birth control, hormone therapy, prolonged sitting or standing, prior deep vein thrombosis and venous valve dysfunction/reflux are all known to increase risk of varicose veins and spider veins. These risk factors lead to increased pressure in the veins known as venous hypertension. The increased pressure from venous hypertension causes the veins close to our skin to stretch and become varicose.
Varicose veins are larger and may bulge and appear rope-like. They often appear on the calf, the back of the leg or inside the thigh. Spider veins are closer to the surface of the skin and look more like thin spider webs. Varicose vein changes can be asymptomatic, but are also associated with symptoms of variable degrees.
Varicose veins can be associated with leg swelling, heaviness, itching and burning, which typically occurs over the day. This creates a state of constant inflammation in the legs, which ultimately damages the skin. In very advanced cases, ulcers can develop in the lower leg around the ankles. They can also be associated with bleeding of fragile veins close to the skin and blood clots.
What You Can Do To Avoid Varicose and Spider Veins
People can take steps on their own to improve blood flow in the legs, keep their legs healthy and help prevent varicose and spider veins, says UH vascular surgeon Karem Harth, MD.
- Get regular physical exercise.
- Lose weight
- Elevate your feet while sitting
- Wear compression stockings
- Avoid prolonged periods of standing/sitting
If you are sitting for long periods of time at work or at home, get up and walk at least every half-hour, Dr. Harth says. Walking is good for vascular health because it helps pump the blood out of the legs and back to the heart by use of our calf muscles. This simple, yet important function, is known as the calf-muscle pump function.
Medical Treatments for Varicose and Spider Veins
Ready To Get Rid of Unsightly Veins?
Our vascular experts can advise you on the optimal therapy for the best results.
Patients seeking treatment for varicose veins often wonder what kinds of therapies are available to them and if these therapies require a significant restrictions in activity during recovery, Dr. Harth says.
“Many surgical and non-surgical treatment options are available, depending on age, overall health, your symptoms and personal preference. These therapies are also primarily offered in the outpatient clinic setting with minimal limitations during recovery and quick return to work,” Dr. Harth says.
Treatments include:
Sclerotherapy: The doctor injects a chemical in the affected veins, which closes off the veins in the area. The veins fade in a few weeks or months. Multiple treatments may be needed. This can be performed for symptomatic small veins close to the skin or for cosmetic reasons.
Laser treatments: For spider veins. Multiple treatments may be needed.
Endovenous ablation: For larger, bulging veins. A doctor inserts a device into the vein and applies heat or glue, which closes it off. Blood is redirected to healthy veins. It may take months for the veins to fade, but symptom relief can be felt days to weeks after the procedure.
Mini-phlebectomy: Varicose veins close to the skin are removed through small incisions.
Surgical ligation and stripping: Performed in rare cases for refluxing veins that are not amenable or have previously failed endovenous ablation therapies. This is done in the operating room.
Related Links
University Hospitals Harrington Heart & Vascular Institute provides diagnosis and treatment of patients with any condition that affects the body’s blood vessels, including varicose veins. With multiple locations across northern Ohio, our providers provides a complete range of services, from routine examinations and medical treatments to the most advanced surgical interventions and post-treatment follow-up for any blood vessel disorder. Learn more about advanced vein care at UH.
Tags: Vascular Disease


